Архив офтальмологии Украины Том 13, №3, 2025
Вернуться к номеру
Нейронспецифічна енолаза у внутрішньоочній рідині як біомаркер стратифікації тяжкості діабетичної ретинопатії
Авторы: Петренко О.В., Литвиненко Т.В.
Національний медичний університет імені О.О. Богомольця, м. Київ, Україна
Рубрики: Офтальмология
Разделы: Клинические исследования
Версия для печати
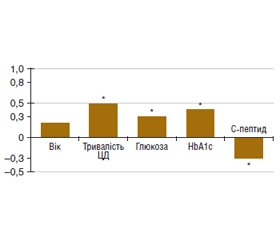
Актуальність. Нейронспецифічна енолаза (NSE) є маркером нейронально-гліального ушкодження. Її локальне вимірювання у внутрішньоочній рідині (ВОР) може відображати градієнт тяжкості діабетичної ретинопатії (ДР) та підсилювати стратифікацію ризику. Мета дослідження: встановити вміст NSE у ВОР та її зв’язок із тяжкістю ДР. Матеріали та методи. Обстежено 110 пацієнтів із цукровим діабетом (ЦД) 2-го типу, яких розподілили на групи за стадією ДР відповідно до Міжнародної класифікації (2003): 1-ша — без ретинопатії (ДР0; 15 очей), 2-га — з початковою непроліферативною ДР (НПДР1; 40 очей), 3-тя — з помірною НПДР (НПДР2; 25 очей), 4-та — з тяжкою НПДР (НПДР3; 12 очей); 5-та — з проліферативною ДР (ПДР; 18 очей). До контрольної групи залучено 25 осіб відповідного віку та статі, які не мали ЦД і ДР. У ВОР, що була отримана під час операції факоемульсифікації катаракти, визначали вміст NSE (мг/мл). Для статистичного аналізу результатів використано пакет EZR v.1.54 (Австрія). Результати. Вік груп був зіставний (p = 0,108), тривалість ЦД зростала зі стадією ДР (p < 0,001). Вміст NSE у ВОР підвищувався від контролю до ПДР (p < 0,001), медіани (мг/мл): контроль — 4,07 (3,42–4,70), ДР0 — 4,66 (4,28–6,23), НПДР1 — 12,28 (10,2–15,4), НПДР2 — 19,20 (16,4–26,9), НПДР3 — 47,63 (42,3–51,6), ПДР — 59,19 (45,6–65,1). Багатокласові межі (мг/мл): < 8,63 (ДР0); 8,63–20,0 (НПДР1); 20,1–40,4 (НПДР2); 40,5–64,0 (НПДР3); > 64,0 (ПДР); для ПДР чутливість 27,8 %, специфічність 100 %; інтегральна точність 0,64 (95% ДІ: 0,56–0,73). Бінаризація (легка/помірна = НПДР1 + НПДР2; тяжка = НПДР3 + ПДР) з порогами 8,27–40,45 та > 40,45 мг/мл забезпечила чутливість/специфічність: 90,8 %/94,3 % (легка/помірна) і 86,7 %/98,1 % (тяжка); інтегральна точність 0,844 (95% ДІ: 0,772–0,901). Висновки. NSE у ВОР відображає градієнт тяжкості ДР і надає клас-специфічні та бінарні пороги для практичної стратифікації (логіка rule-out/rule-in для тяжких форм). Для подальшого впровадження методу потрібна зовнішня валідація.
Background. Neuron-specific enolase (NSE) is a marker of neuronal-glial injury. Its local measurement in the intraocular fluid (IOF) may reflect the gradient of diabetic retinopathy (DR) severity and enhance risk stratification. The purpose of the study was to determine NSE levels in the IOF and their association with DR severity. Materials and methods. We examined 110 patients with type 2 diabetes mellitus who were divided into five groups by the International Clinical Diabetic Retinopathy (2003) classification: group 1 — no retinopathy (DR0; 15 eyes), group 2 — mild non-proliferative DR (NPDR1; 40 eyes), group 3 — moderate NPDR (NPDR2; 25 eyes), group 4 — severe NPDR (NPDR3; 12 eyes), group 5 — proliferative DR (PDR; 18 eyes). The control group included 25 age- and sex-matched individuals without diabetes/DR. In the IOF obtained during phacoemulsification, NSE concentration (mg/mL) was measured. Statistical analysis was performed with EZR v1.54 (Austria). Results. Age was comparable across groups (p = 0.108), while diabetes duration increased with DR stage (p < 0.001). NSE levels in the IOF rose from control to PDR (p < 0.001), medians (mg/mL): control — 4.07 (3.42–4.70), DR0 — 4.66 (4.28–6.23), NPDR1 — 12.28 (10.2–15.4), NPDR2 — 19.20 (16.4–26.9), NPDR3 — 47.63 (42.3–51.6), PDR — 59.19 (45.6–65.1). Multiclass cut-offs (mg/mL): < 8.63 (DR0); 8.63–20.0 (NPDR1); 20.1–40.4 (NPDR2); 40.5–64.0 (NPDR3); > 64.0 (PDR). For PDR, sensitivity was 27.8 %, specificity was 100 %; overall accuracy was 0.64 (95% confidence interval: 0.56–0.73). Binary classification (mild/moderate = NPDR1 + NPDR2; severe = NPDR3 + PDR) with thresholds 8.27–40.45 and > 40.45 mg/mL yielded sensitivity/specificity of 90.8 %/94.3 % (mild/moderate) and 86.7 %/98.1 % (severe); overall accuracy was 0.844 (95% confidence interval: 0.772–0.901). Conclusions. NSE levels in the IOF reflect the DR severity gradient and provide stage-specific and binary thresholds for practical stratification (a rule-out/rule-in logic for severe forms). External validation is required for broader implementation.
діабетична ретинопатія; цукровий діабет 2-го типу; нейронспецифічна енолаза; біомаркери; внутрішньоочна рідина; прогресування захворювання
diabetic retinopathy; type 2 diabetes mellitus; neuron-specific enolase; biomarkers; intraocular fluid; disease progression
Для ознакомления с полным содержанием статьи необходимо оформить подписку на журнал.
- GBD 2019 Blindness and Vision Impairment Collaborators; Vision Loss Expert Group of the Global Burden of Disease Study. Causes of blindness and vision impairment in 2020 and trends over 30 years, and prevalence of avoidable blindness in relation to VISION 2020: the Right to Sight: an analysis for the Global Burden of Disease Study. Lancet Glob Health. 2021 Feb;9(2):e144-e160. doi: 10.1016/S2214-109X(20)30489-7. Epub 2020 Dec 1. Erratum in: Lancet Glob Health. 2021 Apr;9(4):e408. doi: 10.1016/S2214-109X(21)00050-4. PMID: 33275949; PMCID: PMC7820391.
- Magliano DJ, Boyko EJ; IDF Diabetes Atlas 10th edition scien–tific committee. IDF Diabetes Atlas [Internet]. 10th edition. Brussels: International Diabetes Federation; 2021. Available from: https://www.ncbi.nlm.nih.gov/books/NBK581934/.
- Wilkinson CP, Ferris FL 3rd, Klein RE, Lee PP, Agardh CD, Davis M et al.; Global Diabetic Retinopathy Project Group. Proposed international clinical diabetic retinopathy and diabetic macular edema disease severity scales. Ophthalmology. 2003 Sep;110(9):1677-82. doi: 10.1016/S0161-6420(03)00475-5. PMID: 13129861.
- Ong JX, Konopek N, Fukuyama H, Fawzi AA. Deep Capillary Nonperfusion on OCT Angiography Predicts Complications in Eyes with Referable Nonproliferative Diabetic Retinopathy. Ophthalmol Retina. 2023 Jan;7(1):14-23. doi: 10.1016/j.oret.2022.06.018. Epub 2022 Jul 5. PMID: 35803524; PMCID: PMC9813273.
- Nesper PL, Fawzi AA. Perfusion Deficits in Diabetes Without Retinopathy Localize to the Perivenular Deep Capillaries Near the Fovea on OCT Angiography. Ophthalmol Sci. 2024 Feb 1;4(5):100482. doi: 10.1016/j.xops.2024.100482. PMID: 38751454; PMCID: PMC11090878.
- Shinojima A, Lee D, Tsubota K, Negishi K, Kurihara T. Retinal Diseases Regulated by Hypoxia-Basic and Clinical Perspectives: A Comprehensive Review. J Clin Med. 2021 Nov 24;10(23):5496. doi: 10.3390/jcm10235496. PMID: 34884197; PMCID: PMC8658588.
- Lee D, Tomita Y, Miwa Y, Kunimi H, Nakai A, Shoda C, et al. Recent Insights into Roles of Hypoxia-Inducible Factors in Retinal Diseases. Int J Mol Sci. 2024 Sep 21;25(18):10140. doi: 10.3390/ijms251810140. PMID: 39337623; PMCID: PMC11432567.
- Gui F, You Z, Fu S, Wu H, Zhang Y. Endothelial Dysfunction in Diabetic Retinopathy. Front Endocrinol (Lausanne). 2020 Sep 4;11:591. doi: 10.3389/fendo.2020.00591. PMID: 33013692; PMCID: PMC7499433.
- Brooks GA, Arevalo JA, Osmond AD, Leija RG, Curl CC, Tovar AP. Lactate in contemporary biology: a phoenix risen. J Physiol. 2022 Mar;600(5):1229-1251. doi: 10.1113/JP280955. Epub 2021 Feb 25. PMID: 33566386; PMCID: PMC9188361.
- Isgrò MA, Bottoni P, Scatena R. Neuron-Specific Enolase as a Biomarker: Biochemical and Clinical Aspects. Adv Exp Med Biol. 2015;867:125-43. doi: 10.1007/978-94-017-7215-0_9. PMID: 26530364.
- Dunker S, Sadun AA, Sebag J. Neuron specific enolase in re–tinal detachment. Curr Eye Res. 2001 Nov;23(5):382-5. doi: 10.1076/ceyr.23.5.382.5446. PMID: 11910528.
- Abramson DH, Greenfield DS, Ellsworth RM, Fleisher M, Weiss R, Haik B, et al. Neuron-specific enolase and retinoblastoma. Clinicopathologic correlations. Retina. 1989;9(2):148-52. doi: 10.1097/00006982-198909020-00016. PMID: 2772423.
- Nakajima T, Kato K, Kaneko A, Tsumuraya M, Morinaga S, Shimosato Y. High concentrations of enolase, alpha- and gamma-subunits, in the aqueous humor in cases of retinoblastoma. Am J Ophthalmol. 1986 Jan 15;101(1):102-6. doi: 10.1016/0002-9394(86)90471-x. PMID: 3942161.
- Li J, Yan M, Zhang Y, Xie M, Yan L, Chen J. Serum neuron-specific enolase is elevated as a novel indicator of diabetic retino–pathy including macular oedema. Diabet Med. 2015 Jan;32(1):102-7. doi: 10.1111/dme.12597. Epub 2014 Oct 21. PMID: 25252158.
- Asadova V, Gul Z, Buyukuysal RL, Yalcinbayir O. Assessment of neuron-specific enolase, S100B and malondialdehyde levels in serum and vitreous of patients with proliferative diabetic retinopathy. Int Ophthalmol. 2020 Jan;40(1):227-234. doi: 10.1007/s10792-019-01175-9. Epub 2019 Sep 30. PMID: 31571092.
- Yu ZW, Liu R, Li X, Wang Y, Fu YH, Li HY, et al. High Serum Neuron-Specific Enolase Level Is Associated with Mild Cognitive Impairment in Patients with Diabetic Retinopathy. Diabetes Metab Syndr Obes. 2020 Apr 24;13:1359-1365. doi: 10.2147/DMSO.S249126. PMID: 32425568; PMCID: PMC7188072.
- Dolar-Szczasny J, Drab A, Rejdak R. Biochemical Changes in Anterior Chamber of the Eye in Diabetic Patients-A Review. J Clin Med. 2024 Apr 27;13(9):2581. doi: 10.3390/jcm13092581. PMID: 38731110; PMCID: PMC11084197.
- Chu KO, Chan TI, Chan KP, Yip YW, Bakthavatsalam M, Wang CC, et al. Untargeted metabolomic analysis of aqueous humor in diabetic macular edema. Mol Vis. 2022 Aug 19;28:230-244. PMID: 36284671; PMCID: PMC9514551.
- Grochowski ET, Pietrowska K, Godlewski A, Gosk W, Buczynska A, Wojnar M, et al. Simultaneous Comparison of Aqueous Humor and Serum Metabolic Profiles of Diabetic and Nondiabetic Patients Undergoing Cataract Surgery-A Targeted and Quantitative Metabolomics Study. Int J Mol Sci. 2023 Aug 11;24(16):12671. doi: 10.3390/ijms241612671. PMID: 37628855; PMCID: PMC10454064.
- Arai-Okuda M, Murai Y, Maeda H, Kanamori A, Miki T, Naito T, et al. Potentially compromised systemic and local lactate metabolic balance in glaucoma, which could increase retinal glucose and glutamate concentrations. Sci Rep. 2024 Feb 14;14(1):3683. doi: 10.1038/s41598-024-54383-4. PMID: 38355836; PMCID: PMC10866861.
- Lytvynenko TV. Hypoxiainducible factor-α (HIF-1α) and progression of diabetic retinopathy. Medical Science of Ukraine. 2025;3(21):76-84. https://doi.org/10.32345/2664-4738.3.2025.08.
- Sierakowska A, Niewiadomska E, Łabuda S, Bieniasiewicz A, Roszak M, Łabuz-Roszak B. Neuron-Specific Enolase as a Biomarker for Selected Neurological and Psychiatric Disorders — A Systematic Review of the Literature. Medicina (Kaunas). 2025 Oct 13;61(10):1831. doi: 10.3390/medicina61101831.
- Kanda Y. Investigation of the freely available easy-to-use software ‘EZR’ for medical statistics. Bone Marrow Transplant. 2013;48:452-8.
- Brownlee J. One-vs-Rest and One-vs-One for Multi-Class Classification [Internet]. Machine Learning Mastery; 2021 [cited 2025 October 7]. Available from: https://machinelearningmastery.com/one-vs-rest-and-one-vs-one-for-multi-class-classification.
- Robin X, Turck N, Hainard A, Tiberti N, Lisacek F, San–chez J-C, et al. pROC: an open-source package for R and S+ to analyze and compare ROC curves. BMC Bioinformatics. 2011;12(77):1-8. https://doi.org/10.1186/1471-2105-12-77.
- Arya P, Husain N, Kumar C, Shekhar R, Prakash V, Hameed S, et al. C-peptide Level in Patients With Uncontrolled Type 2 Diabetes Mellitus on Oral Anti-diabetic Drugs. Cureus. 2024 Mar 24;16(3):e56810. doi: 10.7759/cureus.56810. PMID: 38654804; PMCID: PMC11036452.
- Hand DJ, Till RJ. A simple generalisation of the area under the ROC curve for multiple class classification problems. Mach Learn. Springer Science and Business Media LLC; 2001 Nov;45(2):171-186.
- Saito T, Rehmsmeier M. The precision-recall plot is more informative than the ROC plot when evaluating binary classifiers on imba–lanced datasets. PLoS One. 2015 Mar 4;10(3):e0118432. doi: 10.1371/journal.pone.0118432. PMID: 25738806; PMCID: PMC4349800.
- Quintyn JC, Pereira F, Hellot MF, Brasseur G, Coquerel A. Concentration of neuron-specific enolase and S100 protein in the subretinal fluid of rhegmatogenous retinal detachment. Graefes Arch Clin Exp Ophthalmol. 2005 Nov;243(11):1167-74. doi: 10.1007/s00417-005-1175-0. Epub 2005 May 20. PMID: 15906069.
- Comoy E, Roussat B, Henry I, Bloch-Michel E. L'énolase neurospécifique dans l'humeur aqueuse. Intérêt dans le diagnostic différentiel du rétinoblastome [Neuron-specific enolase in the aqueous humor. Its significance in the differential diagnosis of retinoblastoma]. Ophtalmologie. 1990 May-Jun;4(3):233-5. French. PMID: 2250954.
- Shine BS, Hungerford J, Vaghela B, Sheraidah GA. Electrophoretic assessment of aqueous and serum neurone-speci–fic enolase in retinoblastoma and ocular malignant melanoma. Br J Ophthalmol. 1990 Jul;74(7):427-30. doi: 10.1136/bjo.74.7.427. PMID: 2378858; PMCID: PMC1042154.
- Yamane K, Minamoto A, Yamashita H, Takamura H, Miyamoto-Myoken Y, Yoshizato K, et al. Proteome analysis of human vitreous proteins. Mol Cell Proteomics. 2003 Nov;2(11):1177-87. doi: 10.1074/mcp.M300038-MCP200. Epub 2003 Sep 15. PMID: 12975481.
- Wang H, Feng L, Hu JW, Xie CL, Wang F. Characterisation of the vitreous proteome in proliferative diabetic retinopathy. Proteome Sci. 2012 Mar 5;10(1):15. doi: 10.1186/1477-5956-10-15. PMID: 22390717; PMCID: PMC3310785.
- Oh JW, Ahn SJ, Jung JH, Kim TW, Kim KP. Proteomic Analysis of Aqueous Humor Identified Clinically Relevant Molecular Targets for Neovascular Complications in Diabetic Retinopathy. Mol Cell Proteomics. 2025 Apr;24(4):100953. doi: 10.1016/j.mcpro.2025.100953. Epub 2025 Mar 19. PMID: 40118382; PMCID: PMC12131854.
- Zhang Y, Xu M, He H, Ren S, Chen X, Zhang Y, et al. Proteomic analysis of aqueous humor reveals novel regulators of diabe–tic macular edema. Exp Eye Res. 2024 Feb;239:109724. doi: 10.1016/j.exer.2023.109724. Epub 2023 Nov 18. PMID: 37981180.
- Pusapati LCV, Padma V, Sathyapriya SV, Nallaperumal S, Vannan I. Association Between Serum Neuron-specific Enolase Levels and Diabetic Neuropathy in Patients With Diabetes Mellitus: A Cross-sectional Study. Cureus. 2025 Jul 3;17(7):e87214. doi: 10.7759/cureus.87214. PMID: 40755599; PMCID: PMC12318130.
- Xie J, Du R, Li Q, Li L. The relationship between neuron-specific enolase, high sensitivity C reactive protein, and diabetic peripheral neuropathy in Chinese patients with type 2 diabetes: A prospective nes–ted case–control analysis. Int J Diabetes Dev Ctries. Springer Science and Business Media LLC; 2024 Mar;44(1):190-199.
- Haque A, Polcyn R, Matzelle D, Banik NL. New Insights into the Role of Neuron-Specific Enolase in Neuro-Inflammation, Neurodegeneration, and Neuroprotection. Brain Sci. 2018 Feb 18;8(2):33. doi: 10.3390/brainsci8020033. PMID: 29463007; PMCID: PMC5836052.
- Sahu S, Nag DS, Swain A, Samaddar DP. Biochemical changes in the injured brain. World J Biol Chem. 2017 Feb 26;8(1):21-31. doi: 10.4331/wjbc.v8.i1.21. PMID: 28289516; PMCID: PMC5329711.
- Zhang J, Sharma D, Dinabandhu A, Sanchez J, Applewhite B, Jee K, et al. Targeting hypoxia-inducible factors with 32-134D safely and effectively treats diabetic eye disease in mice. J Clin Invest. 2023 Jul 3;133(13):e163290. doi: 10.1172/JCI163290. PMID: 37227777; PMCID: PMC10313368.
- Rajala RVS, Rajala A. Unlocking the role of lactate: metabolic pathways, signaling, and gene regulation in postmitotic retinal cells. Front Ophthalmol (Lausanne). 2023 Nov 8;3:1296624. doi: 10.3389/fopht.2023.1296624. PMID: 38983010; PMCID: PMC11182115.
- Lim JI, Kim SJ, Bailey ST, Kovach JL, Vemulakonda GA, Ying GS, et al.; American Academy of Ophthalmology Preferred Practice Pattern Retina/Vitreous Committee. Diabetic Retinopathy Preferred Practice Pattern®. Ophthalmology. 2025 Apr;132(4):P75-P162. doi: 10.1016/j.ophtha.2024.12.020. Epub 2025 Feb 7. PMID: 39918521.
- Brown DM, Wykoff CC, Boyer D, Heier JS, Clark WL, Emanuelli A, et al. Evaluation of Intravitreal Aflibercept for the Treatment of Severe Nonproliferative Diabetic Retinopathy: Results From the PANORAMA Randomized Clinical Trial. JAMA Ophthalmol. 2021 Sep 1;139(9):946-955. doi: 10.1001/jamaophthalmol.2021.2809. PMID: 34351414; PMCID: PMC8343518.
- Maturi RK, Glassman AR, Josic K, Antoszyk AN, Blodi BA, Jampol LM, et al.; DRCR Retina Network. Effect of Intravitreous Anti-Vascular Endothelial Growth Factor vs Sham Treatment for Prevention of Vision-Threatening Complications of Diabetic Retinopathy: The Protocol W Randomized Clinical Trial. JAMA Ophthalmol. 2021 Jul 1;139(7):701-712. doi: 10.1001/jamaophthalmol.2021.0606. PMID: 33784735; PMCID: PMC8010644.
- Berry JL, Xu L, Polski A, Jubran R, Kuhn P, Kim JW, et al. Aqueous Humor Is Superior to Blood as a Liquid Biopsy for Retinoblastoma. Ophthalmology. 2020 Apr;127(4):552-554. doi: 10.1016/j.ophtha.2019.10.026. Epub 2019 Oct 31. PMID: 31767439; PMCID: PMC7093221.
- Castellanos-Canales D, Duffy BV, Decker NL, Yamaguchi TC, Pearce E, Fawzi AA. Relationship of Deep Capillary Plexus Nonperfusion to Visual Acuity and Low Light Vision in Diabetic Retinopathy through OCTA Analysis. Retina. 2025 May 27. doi: 10.1097/IAE.0000000000004517. Epub ahead of print. PMID: 40435504.
- Waheed NK, Rosen RB, Jia Y, Munk MR, Huang D, Fawzi A, et al. Optical coherence tomography angiography in diabetic retino–pathy. Prog Retin Eye Res. 2023 Nov;97:101206. doi: 10.1016/j.pre–teyeres.2023.101206. Epub 2023 Jul 26. PMID: 37499857; PMCID: PMC11268430.
- Yang D, Tang Z, Ran A, Nguyen TX, Szeto S, Chan J, et al. Assessment of Parafoveal Diabetic Macular Ischemia on Optical Coherence Tomography Angiography Images to Predict Diabetic Retinal Disease Progression and Visual Acuity Deterioration. JAMA Ophthalmol. 2023 Jul 1;141(7):641-649. doi: 10.1001/jamaophthalmol.2023.1821. PMID: 37227703; PMCID: PMC10214181.
- Wang T, Chen H, Li N, Zhang B, Min H. Aqueous humor proteomics analyzed by bioinformatics and machine learning in PDR cases versus controls. Clin Proteomics. 2024 May 19;21(1):36. doi: 10.1186/s12014-024-09481-w. PMID: 38764026; PMCID: PMC11103871.
- Ruiz L, Munoz T, González A, Alegre E. Routine data analysis for moderate hemolysis interference correction in neuron specific enolase quantification. Biochem Med (Zagreb). 2025 Jun 15;35(2):020802. doi: 10.11613/BM.2025.020802. PMID: 40520652; PMCID: PMC12161513.
- Nome RV, Paus E, Gehin JE, Bolstad N, Bjøro T. Managing hemolysis in serum neuron-specific enolase measurements - an automated algorithm for routine practice. Scand J Clin Lab Invest. 2024 Jul;84(4):225-229. doi: 10.1080/00365513.2024.2359091. Epub 2024 Jun 10. PMID: 38853575.