Журнал «Здоровье ребенка» Том 21, №1, 2026
Вернуться к номеру
Інтеграція вправ йоги та освітніх занять після пологів знижує рівень кортизолу й показники депресії у матерів із ризиком післяпологової депресії
Авторы: Zahra Azizah Danistya (1), Lilik Herawati (1), Herdika Ayu Retno Kusumasari (2), Budi Prasetyo (1), Sakinah Nuzuliya Izza (1), Mohd Nahar Azmi Mohamed (3)
(1) - Faculty of Medicine, Universitas Airlangga, Indonesia
(2) - Faculty of Medicine, Universitas Brawijaya, Indonesia
(3) - Faculty of Medicine, Universiti Malaya, Malaysia
Рубрики: Педиатрия/Неонатология
Разделы: Клинические исследования
Версия для печати
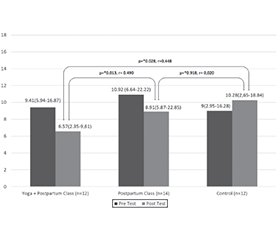
В усьому світі до 20 % матерів, які нещодавно народили, мають післяпологову депресію. В Індонезії її ризик становив від 57,4 до 65 % згідно з Единбурзькою шкалою післяпологової депресії (EPDS). Симптоми депресії супроводжуються високим рівнем кортизолу в крові. Йога та заняття після пологів є синергічними втручаннями, що поєднують фізичну активність і соціальну підтримку. Мета: з’ясувати, чи може йога в поєднанні із заняттями після пологів ефективно запобігати післяпологовій депресії та знижувати рівень кортизолу в крові. Було застосовано квазіекспериментальний дизайн із контрольною групою i вимірюваннями до та після втручання. Останнє проводилося протягом 4 тижнів у 3 групах: комбінація йоги і післяпологових занять (n = 12), тільки післяпологові заняття (n = 14) та відсутність втручання (контрольна група) (n = 12). Усі учасниці мали ≥ 5 балів за шкалою EPDS, що свідчить про ризик розвитку легких симптомів післяпологової депресії. Показники EPDS значно відрізнялися до і після тестування в групі комбінованого втручання з йогою та післяпологовими заняттями (EPDS: p = 0,002, кортизол: p = 0,005), а також у групі лише післяпологових занять (EPDS: p = 0,013), однак без значущих змін біологічного показника (кортизол: p = 0,124). У контрольній групі статистично значущих змін не виявлено (p ≥ 0,05). Поєднання йоги та післяпологових занять було ефективним у зниженні симптомів депресії та рівня кортизолу у післяпологовому періоді.
Up to 20 % of mothers worldwide who have recently given birth experience postpartum depression. In Indonesia, the risk of postpartum depression was 57.4 to 65 % according to the Edinburgh Postpartum Depression Scale (EPDS). Symptoms of depression are accompanied by high blood cortisol levels. Postpartum yoga and postpartum classes are synergistic interventions combining physical activity and social support. This study investigates whether postpartum yoga combined with postpartum classes can effectively prevent postpartum depression and reduce blood cortisol levels. The design employed was a quasi-experimental pretest-post-test control group design. Intervention was carried out over 4 weeks with 3 groups: the combination of yoga + postpartum classes (n = 12), the postpartum classes only (n = 14), and no intervention (controls) (n = 12). All participants had an EPDS score ≥ 5, indicating that the mothers experienced risk of mild postpartum depression symptoms. EPDS and cortisol showed significant differences of pretest and post-test scores in the combined yoga and postpartum class intervention group (EPDS: p = 0.002, cortisol: p = 0.005), and in the postpartum class alone (EPDS: p = 0.013), but not significant in biological parameters (cortisol: p = 0.124), while in the control group, it was not significant (p ≥ 0.05). The combination of yoga and postpartum classes has shown efficacy in managing depression and reducing cortisol levels in postpartum mothers.
післяпологова депресія; йога; післяпологові заняття; кортизол; материнське здоров’я
postpartum depression; yoga; postpartum class; cortisol; maternal health
Для ознакомления с полным содержанием статьи необходимо оформить подписку на журнал.
- McCurdy AP, Boulé NG, Sivak A, Davenport MH. Effects of Exercise on Mild-to-Moderate Depressive Symptoms in the Postpartum Period: A Meta-analysis. Obstet Gynecol. 2017;129(6). Available from: https://journals.lww.com/greenjournal/fulltext/2017/06000/effects_of_exercise_on_mild_to_moderate_depressive.19.aspx.
- Nurbaeti I, Deoisres W, Hengudomsub P. Association between psychosocial factors and postpartum depression in South Jakarta, Indonesia. Sex Reprod Healthc Off J Swedish Assoc Midwives. 2019 Jun;20:72-6.
- Putri AS, Wurisastuti T, Suryaputri IY, Mubasyiroh R. Postpartum Depression in Young Mothers in Urban and Rural Indonesia. J Prev Med Public Health. 2023 May;56(3):272-81.
- Carter T, Bastounis A, Guo B, Jane Morrell C. The effectiveness of exercise-based interventions for preventing or treating postpartum depression: a systematic review and meta-analysis. Arch Womens Ment Health. 2019;22(1):37-53. doi: 10.1007/s00737-018-0869-3.
- Klawetter S, McNitt C, Hoffman JA, Glaze K, Sward A, Frankel K. Perinatal Depression in Low-Income Women: A Literature Review and Innovative Screening Approach. Curr Psychiatry Rep. 2020;22(1):1. doi: 10.1007/s11920-019-1126-9.
- Schiller CE, Meltzer-Brody S, Rubinow DR. The role of reproductive hormones in postpartum depression. CNS Spectr. 2015;20(1):48-59. Available from: https://www.cambridge.org/core/product/AC701DEB8CE0A817B0F68C9BC33A532D.
- Saras T. Hormon: Pesan Keseimbangan dalam Tubuh Manusia. Tiram Media; 2023.
- Kościuszko Z, Sobiński A, Czerwonka M, Kurza K, Kulczycka-Rowicka A, et al. The influence of Hypothalamic-Pituitary-Adrenal (HPA) axis dysregulation on postpartum mental disorders-literature review and new perspectives. Qual Sport. 2025;38:58218.
- Seth S, Lewis AJ, Galbally M. Perinatal maternal depression and cortisol function in pregnancy and the postpartum period: A systematic literature review. BMC Pregnancy Childbirth. 2016;16(1). doi: 10.1186/s12884-016-0915-y.
- Falomo ME, Del Re B, Rossi M, Giaretta E, Da Dalt L, Gabai G. Relationship between postpartum uterine involution and biomarkers of inflammation and oxidative stress in clinically healthy mares (Equus caballus). Heliyon. 2020;6(4):e03691. doi: 10.1016/j.heliyon.2020.e03691.
- Cox EQ, Stuebe A, Pearson B, Grewen K, Rubinow D, Meltzer-Brody S. Oxytocin and HPA stress axis reactivity in postpartum women. Psychoneuroendocrinology. 2015;55:164-72.
- Adams YJ, Miller ML, Agbenyo JS, Ehla EE, Clinton GA. Postpartum care needs assessment: women’s understanding of postpartum care, practices, barriers, and educational needs. BMC Pregnancy Childbirth. 2023;23(1):502.
- Fekadu GA, Ambaw F, Kidanie SA. Facility delivery and postnatal care services use among mothers who attended four or more antenatal care visits in Ethiopia: further analysis of the 2016 demographic and health survey. BMC Pregnancy Childbirth. 2019;19(1):64.
- Saputri Maya E, Selvi Yanti J. Pelaksanaan Kelas Ibu Nifas Sebagai Upaya Peningkatan Kunjungan Ibu Nifas Di Puskesmas Garuda Pekanbaru. Community Engagem Emerg J. 2024;5(2):270-5. Available from: https://journal.yrpipku.com/index.php/ceej.
- Kementrian Kesehatan. Profil Kesehatan. 2024. 100 p.
- Fithriany F, Yuniwati C, Dewi S, Kartika Sari Harahap L. Pengaruh Psikoedukasi Terhadap Kadar Hormon Kortisol Pada Ibu Tujuan Dengan Depresi Postartum Di Wilayah Kerja Dinas Kesehatan Kota Langsa Tahun 2020. J Heal Sains. 2022;3(11):1604-11.
- Shimpuku Y, Iida M, Hirose N, Tada K, Tsuji T, Kubota A, et al. Prenatal education program decreases postpartum depression and increases maternal confidence: A longitudinal quasi-experimental study in urban Japan. Women and Birth. 2022;35(5):e456-63. doi: 10.1016/j.wombi.2021.11.004.
- Inge P, Orchard JJ, Purdue R, Orchard JW. Exercise after pregnancy. Aust J Gen Pract. 2022;51(3):117-21.
- Domínguez-Solís E, Lima-Serrano M, Lima-Rodríguez JS. Non-pharmacological interventions to reduce anxiety in pregnancy, labour and postpartum: A systematic review. Midwifery. 2021 Nov;102:103126.
- Ko YL, Yang CL, Fang CL, Lee MY, Lin PC. Community-based postpartum exercise program. J Clin Nurs. 2013;22(15–16):2122-31.
- Buttner MM, Brock RL, O’Hara MW, Stuart S. Efficacy of yoga for depressed postpartum women: A randomized controlled trial. Complement Ther Clin Pract. 2015;21(2):94-100. doi: 10.1016/j.ctcp.2015.03.003.
- Timlin D, Simpson EEA. A preliminary randomised control trial of the effects of Dru yoga on psychological well-being in Nor–thern Irish first time mothers. Midwifery. 2017;46:29-36. doi: 10.1016/j.midw.2017.01.005.
- Cameron J, Shepherd AL. Evaluation of outcomes from an evidence-based programme for mothers and babies. J Heal Visit. 2018;6(10):499-505.
- Awad MA, Gabre AA, Adly MA, El Refaye GE. Effect of Yoga on Postpartum Depression: A Randomized controlled trial. 2022;21-7.
- Munns L, Spark N, Crossland A, Preston C. The effects of yoga-based interventions on postnatal mental health and well-being: A syste–matic review. Heliyon. 2024;10(3):e25455. doi: 10.1016/j.heliyon.2024.e25455.
- Bershadsky S, Trumpfheller L, Kimble HB, Pipaloff D, Yim IS. The effect of prenatal Hatha yoga on affect, cortisol and depressive symptoms. Complement Ther Clin Pract. 2014 May;20(2):106-13.
- Field T, Diego M, Delgado J, Medina L. Yoga and social support reduce prenatal depression, anxiety and cortisol. J Bodyw Mov Ther. 2013 Oct;17(4):397-403.
- Cox JL, Holden JM, Sagovsky R. Detection of postnatal depression. Development of the 10-item Edinburgh Postnatal Depression Scale. Br J Psychiatry. 1987 Jun;150:782-6.
- Levis B, Negeri Z, Sun Y, Benedetti A, Thombs BD. Accuracy of the Edinburgh Postnatal Depression Scale (EPDS) for screening to detect major depression among pregnant and postpartum women: Systematic review and meta-analysis of individual participant data. BMJ. 2020;371.
- Kusumadewi I, Irawati R, Elvira SD, Wibisono S. Validation study of the Edinburgh postnatal depression scale. Indones Psychiatr Q. 1998;31(2):99-110.
- Sari DN, Diatri H, Siregar K, Pratomo H. Adaptation of the Edin–burgh postnatal depression scale in the Indonesian version: Self-reported anxiety and depression symptoms in pregnant women. Open Access Maced J Med Sci. 2021;9(Dec):1654-9.
- DBC. Database Enzyme-Linked Immunosorbent Assay Cortisol. 2017.
- Dennis C, Dowswell T. Psychosocial and psychological interventions for preventing postpartum depression. Cochrane database Syst Rev. 2013;2.
- Ji Q-Q, Wang M-Y. Epidemiology, pathophysiology, and interventions for postpartum depression: Systematic review. World J Clin Cases. 2025;13(29).
- O’Hara MW, Wisner KL. Perinatal mental illness: definition, description and aetiology. Best Pract Res Clin Obstet Gynaecol. 2014;28(1):3-12.
- Field T, Diego M, Delgado J, Medina L. Tai chi/yoga reduces prenatal depression, anxiety and sleep disturbances. Complement Ther Clin Pract. 2013;19(1):6-10.
- Eustis EH, Ernst S, Sutton K, Battle CL. Innovations in the Treatment of Perinatal Depression: the Role of Yoga and Physical Acti–vity Interventions During Pregnancy and Postpartum. Curr Psychiatry Rep. 2019;21(12):1-9.
- Nakamura A, van der Waerden J, Melchior M, Bolze C, El-Khoury F, Pryor L. Physical activity during pregnancy and postpartum depression: Systematic review and meta-analysis. J Affect Disord. 2019;246:29-41.
- Ruan W, Zhang B, Ma J, Ke H. The Effect of Yoga on Women with Postpartum Depression: A Meta-analysis. Int J Yoga. 2025;18(2):106-14.
- Missler M, van Straten A, Denissen J, Donker T, Beijers R. Effectiveness of a psycho-educational intervention for expecting parents to prevent postpartum parenting stress, depression and anxiety: a randomized controlled trial. BMC Pregnancy Childbirth. 2020;20(1):658.
- Tessema M, Abera M, Birhanu Z. Effectiveness of group-based psycho-education on preventing postpartum depression among pregnant women by primary healthcare provider in primary healthcare institution: a cluster-randomized controlled trial. Front Psychiatry. 2024;15:1433942.
- Carter R, Cust F, Boath E. Peer support workers’ experiences of supporting women with postnatal depression: a constant comparative exploration. J Reprod Infant Psychol. 2018;36(2):168-76.
- King AJ, Simmons MB. A systematic review of the attributes and outcomes of peer work and guidelines for reporting studies of peer interventions. Psychiatr Serv. 2018;69(9):961-77.
- McLeish J, Ayers S, McCourt C. Community-based perinatal mental health peer support: a realist review. BMC Pregnancy Childbirth. 2023;23(1):1-12.
- Oetama EN. Postnatal Counseling on Cortisol Levels and Edin–burgh Postnatal Depression Scale Scores of Postpartum Depression Patients. Pakistan J Life Soc Sci. 2024;22(2):22196-208.
- Sangsawang B, Deoisres W, Hengudomsub P, Sangsawang N. Effectiveness of psychosocial support provided by midwives and fa–mily on preventing postpartum depression among first-time adolescent mo–thers at 3-month follow-up: A randomised controlled trial. J Clin Nurs. 2022;31(5–6):689-702.
- Chaharrahifard L, Motlagh AJ, Akbari-Kamrani M, Ataee M, Esmaelzadeh-Saeieh S. The effect of midwife-led psycho-education on parental stress, postpartum depression and parental competency in high risk pregnancy women: a randomized controlled trial. J Caring Sci. 2021;10(2):70.
- Shorey S, Chan SWC, Chong YS, He HG. A randomized controlled trial of the effectiveness of a postnatal psychoeducation programme on self-efficacy, social support and postnatal depression among primiparas. J Adv Nurs. 2015;71(6):1260-73.
- Oronje S, Kipmerewo M, Okoth J. Outcome of Midwife-Led Debriefing on Postpartum Depression in Western Region, Kenya. Evidence-Based Nurs Res. 2024;6(3):1-10.
- Asadzadeh L, Jafari E, Kharaghani R, Taremian F. Effectiveness of midwife-led brief counseling intervention on post-traumatic stress disorder, depression, and anxiety symptoms of women experiencing a traumatic childbirth: A randomized controlled trial. BMC Pregnancy Childbirth. 2020;20(1):1-9.
- Eskandari B, Nourizadeh R, Mehrabi E, Heshmati R, Ivanbagha R, Akbarivand Z. Evaluating the impact of home supportive counseling and telephone supportive counseling on postpartum depression and anxiety: a randomized controlled trial. BMC Psychiatry. 2025;25(1).
- Franco-Antonio C, Santano-Mogena E, Chimento-Díaz S, Sánchez-García P, Cordovilla-Guardia S. A randomised controlled trial evaluating the effect of a brief motivational intervention to promote breastfeeding in postpartum depression. Sci Rep. 2022;12(1):1-10. doi: 10.1038/s41598-021-04338-w.
- Rodríguez-Gallego I, Vila-Candel R, Corrales-Gutierrez I, Gomez-Baya D, Leon-Larios F. Evaluation of the Impact of a Midwife-Led Breastfeeding Group Intervention on Prevention of Postpartum Depression: A Multicentre Randomised Clinical Trial. Nutrients. 2024;16(2).