Журнал «Медицина неотложных состояний» Том 22, №3, 2026
Вернуться к номеру
Оксидативний стрес, антиоксидантний статус та рівень мікроелементів у пацієнтів з ішемічною хворобою серця в провінції Аль-Мутанна (Ірак)
Авторы: Ali Adil Ajeel
General Directorate of Education Al-Muthanna, Al-Muthanna, Iraq
Рубрики: Медицина неотложных состояний
Разделы: Клинические исследования
Версия для печати
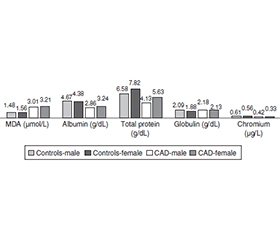
Актуальність. Дослідження включало визначення рівнів деяких параметрів та антиоксидантів у сироватці крові пацієнтів з ішемічною хворобою серця (ІХС) порівняно зі здоровими людьми з метою з’ясування кореляції між цими змінами. Вимірювані параметри включають: малоновий діальдегід (MDA), глутатіон (GSH), вітамін С, сечову кислоту, загальний білок, альбумін, глобулін і деякі мікроелементи (хром (Cr) та селен (Se)). Матеріали та методи. Сироваткові рівні MDA, GSH, вітаміну С, сечової кислоти, загального білка, альбуміну, глобуліну, Cr і Se вимірювали у 100 пацієнтів з ІХС (50 чоловіків, 50 жінок) та 100 умовно здорових осіб (50 чоловіків, 50 жінок). Результати. Статистичний аналіз даних виявив значне підвищення вмісту MDA і сечової кислоти в сироватці крові пацієнтів з ІХС порівняно з контрольною групою. Дослідження також показало суттєве зниження рівнів GSH, Cr та Se в сироватці крові пацієнтів проти контрольної групи і для обох статей. З іншого боку, спостерігалося значне зниження концентрацій вітаміну С, загального білка, альбуміну, тоді як суттєвих відмінностей у рівні глобуліну між пацієнтами та контрольною групою (для обох статей) не виявлено. Висновки. Не було виявлено впливу статі на досліджувані показники, за винятком сечової кислоти.
Background. The study included determination of the levels of some parameters and antioxidants in serum of patients with coronary artery disease (CAD) compared to healthy people aiming at clarifying the relation among these changes. The measured parameters include: malondialdehyde (MDA), glutathione (GSH), vitamin C, uric acid, total protein, albumin, globulin and some trace elements (chromium (Cr) and selenium (Se)). Materials and methods. Serum MDA, GSH, vitamin C, uric acid, total protein, albumin, globulin, Cr and Se were measured in 100 CAD patients (50 male, 50 female) and 100 supposedly healthy subjects (50 male, 50 female). Results. Statistical data analysis revealed a significant elevation in the serum levels of MDA and uric acid in patients with CAD compared to control group. The study also showed a significant decrease in the levels of GSH, Cr and Se in serum of patients as compared to control group and for both sexes. On the other hand, a significant decrease was observed in vitamin C, total protein, albumin, with no significant differences in serum globulin in patients versus control group and for both sexes. Conclusions. There was no effect of sex on the studied parameters except uric acid.
ішемічна хвороба серця; малоновий діальдегід; вітамін С; глутатіон; хром; селен
coronary artery disease; malondialdehyde; vitamin C; glutathione; chromium; selenium
Для ознакомления с полным содержанием статьи необходимо оформить подписку на журнал.
- Frąk W, Wojtasińska A, Lisińska W, Młynarska E, Franczyk B, Rysz J. Pathophysiology of cardiovascular diseases: new insights into molecular mechanisms of atherosclerosis, arterial hypertension, and coronary artery disease. Biomedicines. 2022;10(8):1938.
- Shao C, Wang J, Tian J, Tang Y. Coronary artery disease: from mechanism to clinical practice. Coron Artery Dis Ther Drug Discov. 2020;1-36.
- Russo M, Gurgoglione FL, Russo A, Rinaldi R, Torlai Triglia L, Foschi M, et al. Coronary artery disease and atherosclerosis in other vascular districts: Epidemiology, risk factors and atherosclerotic plaque features. Life. 2025;15(8):1226.
- Agrawal A, Lamichhane P, Eghbali M, Xavier R, Cook DE, Elsherbiny RM, et al. Risk factors, lab parameters, angiographic characteristics and outcomes of coronary artery disease in young South Asian patients: a systematic review. J Int Med Res. 2023;51(8):03000605231187806.
- Dos Santos CCL, Matharoo AS, Cueva EP, Amin U, Ramos AAP, Mann NK, et al. The influence of sex, age, and race on coronary artery disease: a narrative review. Cureus. 2023;15(10).
- Pintos-Rodríguez S, Jiménez Díaz VA, Veiga C, Martínez García C, Caamaño Isorna F, Íñiguez Romo A, et al. Coronary artery disease in very young women: risk factors and prognostic insights from extended follow-up. J Cardiovasc Dev Dis. 2025;12(2):34.
- Duggan JP, Peters AS, Trachiotis GD, Antevil JL. Epidemiology of coronary artery disease. Surg Clin. 2022;102(3):499-516.
- Nweke M, Ibeneme S, Pillay JD, Mshunqane N. Characterization and risk stratification of coronary artery disease in people living with HIV: a global systematic review. Front Cardiovasc Med. 2025;12:1586019.
- Mujtaba A, Rehman M, Ali Ja, Zafar B, Tammar M, Meh–mood A, et al. Assessment of risk factors for coronary artery disease in patients attending a tertiary care hospital: a cross-sectional study. Insights-Journal Heal Rehabil. 2025;3(3):87-94.
- Boden WE, De Caterina R, Kaski JC, Bairey Merz N, Berry C, Marzilli M, et al. Myocardial ischaemic syndromes: a new nomenclature to harmonize evolving international clinical practice guidelines. Eur Heart J. 2024;45(36):3701-6.
- Kittleson MM. Chronic coronary artery disease. Ann Intern Med. 2025;178(10):ITC145-60.
- Luo C, Tong Y. Comprehensive study and review of coronary artery disease. In: Second International Conference on Biological Engineering and Medical Science (ICBioMed 2022). SPIE; 2023. 502-8.
- Al-Salih RMH, Ali ZM. Relations between Interleukin-6 and Some Biochemical Parameters in Diabetic Foot Syndrome. Medico-Legal Updat. 2021;21(1).
- Asmat U, Abad K, Ismail K. Diabetes mellitus and oxidative stress — A concise review. Saudi Pharm J. 2016;24(5):547-53.
- Oparil S, Zaman MA, Calhoun DA. Pathogenesis of hypertension. Ann Intern Med. 2003;139(9):761-76.
- Sies H. Oxidative stress: concept and some practical aspects. Antioxidants. 2020;9(9):852.
- Wolin MS, Gupte SA. Novel roles for NOX oxidases in cardiac arrhythmia and oxidized glutathione export in endothelial function. Vol. 97, Circulation research. Lippincott Williams & Wilkins; 2005. 612-4.
- Poli G, Leonarduzzi G, Biasi F, Chiarpotto E. Oxidative stress and cell signalling. Curr Med Chem. 2004;11(9):1163-82.
- De Champlain J, Wu R, Girouard H, Karas M, El Midaoui A, Laplante M, et al. Oxidative stress in hypertension. Clin Exp Hypertens. 2004;26(7–8):593-601.
- Madamanchi NR, Vendrov A, Runge MS. Oxidative stress and vascular disease. Arterioscler Thromb Vasc Biol. 2005;25(1):29-38.
- Pillai CK, Pillai KS. Antioxidants in health. Indian J Physiol Pharmacol. 2002.
- Sam F, Kerstetter DL, Pimental DR, Mulukutla S, Tabaee A, Bristow MR, et al. Increased reactive oxygen species production and functional alterations in antioxidant enzymes in human failing myocardium. J Card Fail. 2005;11(6):473-80.
- Katoch N, Kaur P, Kashyap P, Gupta S, Dahiya RS. Role of oxidative stress in cardiovascular diseases. Research Journal of Pharmaceutical, Biological and Chemical Sciences. 2013;4(3).
- Viitala PE, Newhouse IJ, LaVoie N, Gottardo C. The effects of antioxidant vitamin supplementation on resistance exercise induced lipid peroxidation in trained and untrained participants. Lipids Health Dis. 2004;3(1):14.
- LaMonte MJ, Eisenman PA, Adams TD, Shultz BB, Ainsworth BE, Yanowitz FG. Cardiorespiratory fitness and coronary heart disease risk factors: the LDS Hospital Fitness Institute cohort. Circulation. 2000;102(14):1623-8.
- Girotti AW. Mechanisms of lipid peroxidation. J Free Radic Biol Med. 1985;1(2):87-95.
- Halliwell B, Gutteridge Jm. Oxygen toxicity, oxygen radicals, transition metals and disease. Biochem J. 1984;219(1):1.
- Young IS, McEneny J. Lipoprotein oxidation and atherosclerosis. Biochem Soc Trans. 2001;29(2):358-62.
- Caimi G, Carollo C, Lo Presti R. Diabetes mellitus: oxidative stress and wine. Curr Med Res Opin. 2003;19(7):581-6.
- Rahman K. Studies on free radicals, antioxidants, and co-factors. Clin Interv Aging. 2007;2(2):219-36.
- Matés JM, Pérez-Gómez C, De Castro IN. Antioxidant enzymes and human diseases. Clin Biochem. 1999;32(8):595-603.
- Kalpravidh RW, Wichit A, Siritanaratkul N, Fucharoen S. Effect of coenzyme Q10 as an antioxidant in β-thalassemia/Hb E patients. Biofactors. 2005;25(1–4):225-34.
- Diplock AT, Charuleux JL, Crozier-Willi G, Kok FJ, Rice-Evans C, Roberfroid M, et al. Functional food science and defence against reactive oxidative species. Br J Nutr. 1998;80(S1):S77-112.
- Maltais D, Desroches D, Aouffen M, Mateescu MA, Wang R, Paquin J. The blue copper ceruloplasmin induces aggregation of newly differentiated neurons: a potential modulator of nervous system organization. Neuroscience. 2003;121(1):73-82.
- Ellman GL. Tissue sulfhydryl groups. Arch Biochem Biophys. 1959;82(1):70-7.
- Tietz NW, Andresen BD. Textbook of clinical chemistry. 1986.
- Burtis CA, Ashwood ER, Tietz NW. Tietz textbook of clinical chemistry. 1999.
- Doumas BT, Biggs HG, Arends RL, Pinto PVC. Determination of serum albumin. In: Standard methods of clinical chemistry. Elsevier; 1972. 175-88.
- Li Pomi F, Gammeri L, Borgia F, Di Gioacchino M, Gangemi S. Oxidative Stress and Skin Diseases: The Role of Lipid Peroxidation. Antioxidants. 2025;14(5):555.
- Akbari B, Najafi F, Bahmaei M, Mahmoodi NM, Sherman JH. Modeling and optimization of malondialdehyde (MDA) absorbance behavior through response surface methodology (RSM) and artificial intelligence network (AIN): An endeavor to estimate lipid peroxidation by determination of MDA. J Chemom. 2023;37(4):e3468.
- Hadi N, Zaidi IA, Kamal Z, Khan RU, Khan MH, Omair F, et al. Estimation of Serum Malondialdehyde (a Marker of Oxidative Stress) as a Predictive Biomarker for the Severity of Coronary Artery Disease (CAD) and Cardiovascular Outcomes. Cureus. 2024;16(9).
- Sadeghi N, Abedi H, Atashpour S, Etemadi S. Antioxidant Mechanisms in Myocardial Ischemia: Narrative Review. Multidiscip Cardiovasc Ann. 2023;14(2).
- Sarhat ER, Mohammed IJ, Mohammed NY, Khairy BS, Hassan GF. Evaluation of salivary oxidative stress marker (lipid peroxidation), and non-enzymatic antioxidants (vitamin c and vitamin e) in patients with acute myocardial infarction. Tikrit J Dent Sci. 2019;7(1):20-6.
- Ahmed I, Khan H, Afroz N, Diwayo A, Ahmed J. Serum Oxidative Stress Biomarkers and Antioxidant Enzyme Activity as Predictors of Cardiovascular Risk in Patients with Type 2 Diabetes Mellitus: Oxidative Stress, Antioxidants, and Cardiovascular Risk in T2DM. Dev Medico-Life-Sciences. 2025;2(7):16-21.
- Burgeiro A, Santos D, Fonseca ACRG, Baldeiras I, Leal EC, Moura J, et al. Enhanced Mitochondrial Dynamics and Reactive Oxygen Species Levels with Reduced Antioxidant Defenses in Human Epicardial Adipose Tissue. Metabolites. 2025;15(7):481.
- Al-Lami NJK, Awad NAN, Al-Taher SSH. Clinical study on the relationship between exposure to ultrafine particles (PM0.1) and cardiovascular diseases in petroleum workers. Toxicol Reports. 2025;102119.
- Zhou Z, Zhang Y, Zhao R, Liu D, Xie B, Zhang Q, et al. Mitochondrial Oxidative Stress and Cardiac Dysfunction in TERT Deficient Progeria Mice. Clin Exp Pharmacol Physiol. 2025;52(12):e70082.
- Wei T, Wang Q, Chen T, Zhou Z, Li S, Li Z, et al. The possible association of mitochondrial fusion and fission in copper deficiency-induced oxidative damage and mitochondrial dysfunction of the heart. J Trace Elem Med Biol. 2024;85:127483.
- Moronkeji AI, Olaniyan MF. Evaluation of 8-hydroxy-2’-deoxyguanosine, interleukin-8 and malondialdehyde among patients with cardiovascular diseases in Ibadan, Oyo State. Sokoto J Med Lab Sci. 2024;9(2):160-9.
- Tsikas D, Tsikas SA, Mikuteit M, Ückert S. Circulating and urinary concentrations of malondialdehyde in aging humans in health and disease: review and discussion. Biomedicines. 2023;11(10):2744.
- Zheng H, Xu Y, Liehn EA, Rusu M. Vitamin C as scavenger of reactive oxygen species during healing after myocardial infarction. Int J Mol Sci. 2024;25(6):3114.
- Athanasiou A, Charalambous M, Anastasiou T, Aggeli K, Soteriades ES. Preoperative and postoperative administration of vitamin C in cardiac surgery patients — settings, dosages, duration, and clinical outcomes: a narrative review. Ann Med Surg. 2024;86(6):3591-607.
- Jin S, Kang PM. A systematic review on advances in management of oxidative stress-associated cardiovascular diseases. Antioxidants. 2024;13(8):923.
- Młynarska E, Biskup L, Możdżan M, Grygorcewicz O, Możdżan Z, Semeradt J, et al. The role of oxidative stress in hypertension: the insight into antihypertensive properties of vitamins A, C and E. Antioxidants. 2024;13(7):848.
- Nsairat H, Lafi Z, Abualsoud BM, Al-Najjar BO, Al-Samydai A, Oriquat GA, et al. Vitamin C as a Cardioprotective Agent Against Doxorubicin-Induced Cardiotoxicity. J Am Heart Assoc. 2025;14(16):e042534.
- Chen TH, Wang HC, Chang CJ, Lee SY. Mitochondrial glutathione in cellular redox homeostasis and disease manifestation. Int J Mol Sci. 2024;25(2):1314.
- De Medina M, Ashby M, Diego J, Pennell JP, Hill M, Schiff ER, et al. Factors that influence serum hyaluronan levels in hemodialysis patients. ASAIO J. 1999;45(5):428-30.
- Czinege M, Ruța F, Nyulas V, Halațiu VB, Nyulas T, Benedek T. Serum albumin concentration and the risk of cardiovascular disease and acute coronary syndrome — a narrative review. J Cardiovasc Emergencies. 2025;11(1):11-9.
- Shimada BK, Alfulaij N, Seale LA. The impact of selenium deficiency on cardiovascular function. Int J Mol Sci. 2021;22(19):10713.
- Ekpenyong CE. Essential trace element and mineral deficiencies and cardiovascular diseases: facts and controversies. Int J Food Sci Nutr. 2017;6:53-64.
- Leszto K, Biskup L, Korona K, Marcinkowska W, Możdżan M, Węgiel A, et al. Selenium as a modulator of redox reactions in the prevention and treatment of cardiovascular diseases. Antioxidants. 2024;13(6):688.
- Dabravolski SA, Sukhorukov VN, Melnichenko AA, Khotina VA, Orekhov AN. The role of selenium in atherosclerosis development, progression, prevention and treatment. Biomedicines. 2023;11(7):2010.
- Ye Y, Liao G, Liu T, Hu X, Chen X, Bai L, et al. Allopurinol for secondary prevention in patients with cardiovascular disease: a systematic review and meta-analysis of randomized controlled trials. J Cardiovasc Dev Dis. 2023;10(9):379.
- Mackenzie IS, Hawkey CJ, Ford I, Greenlaw N, Pigazzani F, Rogers A, et al. Allopurinol and cardiovascular outcomes in patients with ischaemic heart disease: the ALL-HEART RCT and economic evaluation. Health Technol Assess. 2024;28(18):1.