Журнал «Медицина неотложных состояний» 2 (57) 2014
Вернуться к номеру
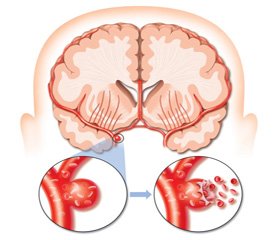
Acute neurotrophic disorders of the digestive system against the background of a cerebral stroke
Авторы: Saiko O.V. — Military Medical Clinical Centre West region, Lviv
Рубрики: Медицина неотложных состояний
Версия для печати
stroke, acute neurotrophic disorders: calculous cholecystitis, bile peritonitis, ulcer, hemorrhage, pancreatitis, pancreatic necrosis.
Neurological disorders accompanied by the development of extracerebral diseases in all patients with severe acute cerebral stroke. It often comes to the fore and lead to death.There are five most common types of acute extracerebral pathologies that determine the progress of stroke and influence its outcome, regardless of the nature and location: acute pathology of the respiratory and cardiovascular system, pulmonary embolism, urinary tract pathology and pathology of the gastrointestinal tract.Acute pathology of the digestive system is represented by acute changes of the mucosa of the esophagus, ulcers and erosion of the stomach or duodenal mucosa, gastrointestinal bleedings, intestinal obstruction and dynamic enterocolitis, Malory-Weiss syndrome, pancreatic encephalopathy with the development of pancreatic necrosis and "pancreatic shock", all morphological forms of acute cholecystitis, purulent cholangitis. Extracerebral pathology in severe forms of cerebral stroke suddenly occurs at the level of individual organs or systems. Violations of regulatory and trophic effects of brain as a result of direct or indirect effects on cerebral-visceral connections, hypothalamic-pituitary area, the structures of the limbic system, and the centers regulating vital functions in the brain stem should be considered the leading element of the pathogenesis of extracerebral complications of cerebral stroke. Thus violation of visceral nervous system and endocrine system regulation play a key role in the development of pathology of extracerebral stroke. Rapid activation of sympathetic-adrenal system and hypothalamic-pituitary-adrenal system leads to increased release into the bloodstream of glucocorticoids, mineralocorticoids and catecholamines. Rapid activation of the sympathetic-adrenal system and hypothalamic-pituitary-adrenal system leads to an increase in the release of blood glucocorticoids, mineralocorticoids and catecholamines. After breach of the hematoencephalic barrier, structural and functional changes in stroke trigger both local and systemic inflammatory response. Central impairment of the regulation of cellular and humoral immunity leads to hyperactivation or depression of the immune response. Thus, violation of coordinating and regulatory functions of the CNS can be considered as the leading pathogenetic mechanism of extracerebral changes. Initially emergence or exacerbation of illnesses of the internal organs appear against the background of a stroke, and also as a result of intensive treatment. Consequently, a number of sudden-onset diseases of internal organs is an aggravation of chronic diseases that occurred in the development of stroke and can lead to death. Therefore, practicing physicians-neurologists, neuro-reanimatologists based on the obtained anamnestic, clinical, and laboratory and instrumental data, can predict the occurrence of sudden extracerebral complications of acute cerebrovascular accidents, and choose the right tactics to prevent their probable onset, and in appearance — treatment.