Журнал «Боль. Суставы. Позвоночник» 3 (15) 2014
Вернуться к номеру
Is TBS different in healthy European caucasian men and women? Creation of normative spine TBS data for men
Авторы: Povoroznyuk V.V. - State Institution «Institute of Gerontology named after D.F. Chebotarev of National Academy of Medical Sciences of Ukraine», Kyev, Ukraine; Del Rio L., Di Gregorio S. - Cetir Group Mèdic, Barcelona, Spain; Michelet F. - R&D department, Med-Imaps, France; Dzerovych N., Musiienko A. - State Institution «Institute of Gerontology named after D.F. Chebotarev of National Academy of Medical Sciences of Ukraine», Kyev, Ukraine; Winzenrieth R. - R&D department, Med-Imaps, France
Рубрики: Ревматология, Травматология и ортопедия
Разделы: Новости
Версия для печати
Статья опубликована на с. 20-23
Introduction
Trabecular Bone Score (TBS iNsight v2.1, Med-Imaps, France) is an index of bone microarchitectural texture extracted from antero-posterior spine DXA.
Normative data for TBS are already published for French and US non-Hispanic White women elsewhere [1]. It has been observed that TBS values for all lumbar vertebral combinations decreased significantly with age. There was a linear decrease of 16.0 % (–2.47 and –2.58 T-score for US and French data) in TBS at L1–L4 between 45 and 90 yr of age. Microarchitectural loss rate increased after age 65 by 50 % (0.004 to 0.006) in both data set. The changes we observed in these American women are similar to that reported for a French population of white women (r2 = 0.99). However, no data exist concerning TBS in men.
Objective
In this cross-sectional analysis from two facilities in Ukraine and Spain, we have investigated the age-related changes of the lumbar vertebrae microarchitecture assessed by TBS in a cohort of Caucasian men.
Patient & methods
Population
The population of study was constituted from databases of two densitometer systems from two different clinical centers. The men subjects were selected in lists of patients from:
— Cetir Group Mèdic, Barcelona, Spain;
— Department of Clinical Physiology & Pathology of Locomotor Apparatus, D.F. Chebotarev Institute of Gerontology NAMS, Ukraine and Ukrainian Scientific-Medical Center for the Problems of Osteoporosis, Kiev, Ukraine.
With age ranged between 40 and 90 years. From these two centers a cohort of 368 White European Caucasian men was created using the normative data protocol (MEN-Study protocol.doc). A wide range of BMI was studied from 17 to 36 kg/m2. Subjects with higher BMI were excluded because they did not represent a normal patient. Participants were divided into five groups by decade: 40–50, 50–60, 60–70, 70–80, 80–90 with a minimum of 25 subjects per decade.
Method
BMD was evaluated with two DXA fan-beam bone densitometers (a Prodigy and a iDXA, GE-LUNAR, Madison, WI, USA) at spine. Antero-Posterior (AP) spine acquisitions were used. BMD assessment was done at L1–L4. TBS was evaluated in the same regions of measurement as those used for BMD using TBS Clinical Data analyzer V2.1.0.2 (Med-Imaps). TBS was calculated as the mean value of the individual measurements for each vertebra and their combinations from L1 through L4.
The two centers were cross calibrated for TBS using a linear regression equations. The center of Barcelona was cross-calibrated to the Kiev center.
For each subject, the following parameters were determined from patient files and records of the DXA exam: clinical records as described in the normative data protocol (MEN-Study protocol.doc), patient age, weight, height and body mass index (BMI), BMD, for each vertebra and their combinations from L1 through L4. Each set of clinical data, DXA measurements and the TBS were imported into an Excel file. All data from these subjects were first anonymized before inclusion in the study.
Statistical Analysis
Statistical analysis was carried out by age group using Medcalc and Excel softwares. Descriptive statistics were performed in order to characterize the population of study. Association between continuous variables was assessed by Pearson's correlation coefficient. Age-related curves for TBS were created using Excel solver and multiple regressions. The generalized reduced gradient approach was used which is a non linear optimization algorithm. The end point of the optimization was to minimized the sum of the squarred errors between data and predicted values. FA P-value < 0.05 was considered statistically significant.
Results
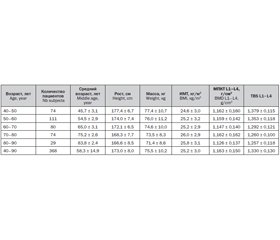
A database of 368 men aged 40 to 90 years was created (table 1).
TBS and BMD values at L1–L4 were poorly correlated with BMI (r = 0.16 and r = 0.22). TBS was poorly correlated with weight (r = –0.1) and height (0.03) whereas higher correlations were obtained for BMD (r = 0.3 and r = 0.2).
TBS values obtained for all lumbar vertebral combinations decreased significantly with age (fig. 1, at L1–L4 for men and women). TBS values obtained for all lumbar vertebral combinations (L1, L2, L3, L4) decreased significantly with age in men.
There was a linear decline of 13.5 % (–1.75 T-score) in TBS at L1–L4 between 40 and 90 years of age in men whereas a decline of 16.7 % (~–2.58 T-score) was observed in women (Dufour et al., OI 2012). Conversely to women, it seems that there is no modification of TBS decline rate after 65 years in men.
Conclusion
— This study established for the first time TBS age related curve in European men at lumbar spine.
— The decrease seen in lumbar TBS reflects age-related micro-architecture texture changes at spine.
— Within 40-65 age range, similar TBS decline was observed in both European Caucasian men and women (p = 0.8). After 65, TBS decline rate is significantly higher for women than for men (p < 0.01).
— This study confirms the need for using gender dedicated reference data.
1. Generation and validation of normative, age-speci–fic reference curve for lumbar spine trabecular bone score (TBS) in French women / Dufour R., Winzenrieth R., Heraud A., Hans D., Mehsen N. // Osteoporos Int. — 2013 Nov. — 24(1). — 2837-46.

/22/22.jpg)
/22/22_2.jpg)