Журнал «Здоровье ребенка» 8 (59) 2014
Вернуться к номеру
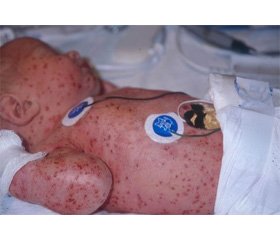
Langerhans cell hystiocytosis in child of young age
Авторы: N.N. Kaladze, A.V. Yurieva, L.D. Gafarova - PI «Crimean State University named after S.I. Georgievskiy»; V.A. Filimonenkova - The Crimean Republican institution «Children’s Clinical Hospital»; T.I. Shipunova, A.S. Pysarenko - City children''s Clinical Hospital № 3, Simferopol
Рубрики: Педиатрия/Неонатология
Разделы: Справочник специалиста
Версия для печати
Modern classification of histiocytosis includes threе nosological forms: Langerhans cell histiocytosis, malignant histiocytosis and virus-associated hemophagocytic syndrome. Langerhans cell histiocytosis mainly affects children under 15 years old and it affects boys more than girls. The average age at the moment of diagnosis is about 3 years old. The clinical manifestations are diverse, which make the diagnosis difficult. Late diagnosis increases the chance of developing diabetes insipidus and/or stunted growth in a patient. The submitted clinical case of Langerhans cells histiocytosis is an example of late diagnosis (with developed complications) and a complex diagnostic search when trying to diagnose. The boy G., 3 years 2 months old, was enrolled to endocrinology department of City Children's Clinical Hospital № 3 in Simferopol to pediatric endocrinologist with complaints of weight loss, frequent urination, especially at night (4-5 times per night), thirst (more than 3 liters of fluid per day), a tendency to constipation, intermittent cough, impaired nasal breathing. The preliminary diagnosis on admission was diabetes insipidus. The peculiarities of the anamnesis were as following: the boy was seen by a neurologist about hydrocephalus until the age of one; during the last year he had been treated by a dermatologist about seborrheic dermatitis, at 2 years and 8 months of age he had the obstructive bronchitis, at 3 years of age he had ARVI, at 3 years of age - DTP-polio booster dose. The child’s well-being had deteriorated during the last months when the mentioned symptoms appeared. On the day of treatment to the local doctor he was examined by an endocrinologist, a urine specific gravity was 1001; the child was sent to the hospital. At the time of admission he had a state of moderate severity, the skin was pale and dry, the turgor was decreased, there were dark circles under his eyes and his lips were dry. The patient had difficulty breathing through the nose. The entire scalp was oozing, covered with crusts and traces of scratching. Hydrocephalic shape of the head, ptosis of the eyelids and appetite loss were observed. Liver increased by 2.5 cm, spleen was not palpable. Cardiovascular system had no symptoms. The breathing over the lungs was harsh without crepitation and lung sounds were heard on percussion. The child had a high urine output, nocturia and nocturnal enuresis. Bowel movements occurred once every 2 - 3 days and was formed. The level of β-lipoproteins in the blood was increased. Urine specific gravity was 1005, daily urine output was 3,200 mL. Nocturia and hyposthenuria were present. The conclusion of the professionals: a dermatologist - gneiss, an allergist - seborrheic dermatitis with eczematization, an ENT - allergic rhinitis and wax plugs. Radiography of the skull in the sagittal plane showed that there was a claviform shade of the medium intensity over the anterior and middle cranial fossae. Radiography of the ephippium and thorax organs had no pathology. CT scan of the brain showed that there were a defected area, 17x25mm in size, on the right of the greater wing of the sphenoid bone anterior to the foramen ovale and a defected area, 16x20 mm in size, left to the superior side of the orbit and at the same level there was a defected area, 5x6 mm in size, in the frontal squama. The margins of the bone defects were wavy and distinct. There were sacs of soft-tissue density in the area of the defects. Focal changes in the brain hadn’t been revealed. CT didn`t reveal the signs of pituitary microadenoma. On the basis of the above data was diagnosed Langerhans cell histiocytosis, central diabetes insipidus of moderate severity. The treatment by uropres was started with the dosage of 5 mcg in the morning and in the evening, under the control of diuresis. On the 4th day the child was counsulted by the oncohematologist of the Crimean Republican institution ‘Children’s Clinical Hospital’ and the next day he was admitted to the Oncohematological Department of CRI ‘CCH’ for further examination and treatment. In the hospital the diagnosis was confirmed and the therapy according to the protocol LCH-III, the initial course, the standard supporting therapy and the prevention of the desmopressin replacement therapy were carried out. The positive dynamics were observed in absence of bone defects and in normal level of histiocytes. Thus, today the problem of timely diagnosis of histiocytosis, which determines the severity of complications and prognosis of the disease, for the doctors who see the patient first, e.g. pediatricians and family doctors, is relevant. Family doctors and pediatricians should suspect the presence of Langerhans cell histiocytosis when the following symptoms are present: seborrheic dermatitis of the scalp; xanthelasmatosis; chronic otitis, mastoiditis; fever of unknown origin with enlarged lymph nodes, liver and spleen, excluding hemoblastosis; swollen lymph nodes, and / or liver and / or spleen excluding liver diseases and hematological malignancies; disseminated lung affection, "honeycomb lung"; centers of osteolysis on the radiography (except bones of the hand and foot); exophthalmos except endocrine diseases other than diabetes insipidus; diabetes insipidus. When examining the patient with a combination of the above symptoms and suspecting histiocytosis, the doctor should provide modern morphological verification of the diagnosis and prompt and intensive treatment that can achieve stable remission, reduce the risk of recurrence and improve the prognosis of the disease up to complete recovery.