Статтю опубліковано на с. 27-30
Вступ
Захворювання органів дихання залишаються актуальною медико-соціальною проблемою, що пов’язано з їх високою частотою, складністю діагностики, ризиком формування хронічної респіраторної патології, що призводить до інвалідизації.
Захворювання органів дихання мають домінуюче положення в структурі захворюваності дітей. Так, частота бронхітів коливається в межах 7,5–25 %, пневмоній — 5–12 % [6]. У нозологічній структурі гострих бронхітів у дітей на обструктивні бронхіти припадає близько 20–25 %, частіше такий варіант перебігу бронхіту реєструється у дітей раннього віку, що певною мірою обумовлено анатомо-фізіологічними особливостями, факторами преморбідного фону, станом імунної системи та характером відповіді макроорганізму [2, 5].
За офіційними даними, в Україні за останні 10 років питома вага дітей, які часто хворіють на гострі респіраторні захворювання (ГРЗ), зросла до 50–90 %. Встановлено, що сприятливий прогноз при захворюваннях органів дихання у дітей залежить від ранньої діагностики й адекватної етіотропної терапії. При цьому своєчасне їх виявлення базується на результатах детального та послідовного аналізу клініко-анамнестичних і рентгенологічних даних.
Літературний огляд
Провідними клінічними симптомами, що дозволяють запідозрити у дитини бронхолегеневу патологію, є: інтоксикація, лихоманка, кашель, утруднення дихання, ціаноз і типові фізикальні дані над легенями. Для ГРЗ провідним є температура тіла < 38 °С з тенденцією до її нормалізації протягом трьох днів. При пневмонії температура тіла > 38 °С із тривалістю понад 3 дні (виняток — атипові форми в перші місяці життя), тоді як при бронхітах зазвичай температура тіла буває < 38 °С або вона протягом 1–3 днів знижується до цього рівня [1, 4].
Перше завдання в діагностиці — виявити у дитини з ознаками ГРЗ ураження нижніх дихальних шляхів, для яких характерною є наявність хоча б однієї з таких ознак: задишка з утрудненням (обструкцією) дихання, скорочення перкуторного звуку, наявність вологих хрипів різного калібру.
Друге завдання — відрізнити пневмонію від бронхіту, переважно вірусного ураження верхніх дихальних шляхів. Важливий симптом пневмонії — збільшення частоти дихання, що спостерігається тим частіше, чим більше площа ураження легень і чим менший вік дитини. Проте ця ознака значуща тільки за відсутності симптомів обструкції, що характерна для крупу і бронхітів, у тому числі обструктивного. Параметри частоти дихання (за 1 хв), за даними ВООЗ, характерні для пневмонії, становлять понад 60 у дітей віком 0–2 міс., понад 50 у дітей віком 2–12 міс., понад 40 — у дітей віком 1–4 роки [7].
Скорочення перкуторного звуку також характерно для пневмонії, але зустрічається лише в половини випадків, тому його відсутність сьогодні не виключає пневмонії. Це стосується і локалізованих над місцем ураження дрібнопухирчастих або крепітуючих хрипів та ослабленого або бронхіального дихання. Їх виявлення дозволяє встановити діагноз пневмонії, але відсутність їх такий діагноз не виключає. У половини всіх хворих із типовою пневмонією в гострому періоді хрипи можуть бути відсутні. Хрипи, що рівномірно вислуховуються в обох легенях, як і обструкція, характерні для бронхітів, але не для пневмонії: сухі хрипи виявляються у 10 %, а розсіяні вологі — у 25 % хворих, найчастіше вони асиметричні [3].
Оскільки діагноз пневмонії за вказаними вище фізикальними даними вдається встановити менше ніж у половини випадків, слід використовувати алгоритм, створений на підставі запропонованих ВООЗ ознак. Алгоритм звільняє педіатра від необхідності встановлювати діагноз при нестачі інформації й дозволяє знизити гіпердіагностику пневмонії і скоротити клькість необґрунтованих рентгенівських знімків і призначень антибіотиків; його чутливість — 94 %, специфічність — 95 % [7].
Якою мірою допомагають діагностиці лабораторні дані? Лейкоцитоз 10–15 • 109/л спостерігається в перші дні у половини хворих на пневмонію, але також і у третини хворих на ГРЗ, гострий бронхіт. Так що сам по собі він не свідчить про бактеріальну інфекцію і не вимагає призначення антибіотиків. Але й число лейкоцитів нижче від 10 • 109/л у ряді випадків не виключає пневмонії. Це може бути характерно для пневмоній, викликаних гемофільною паличкою і мікоплазмою, а також нерідко спостерігається при пневмонії в перші дні хвороби іншої етіології. Цифри лейкоцитозу вище від 15 • 109/л (і/або абсолютне число нейтрофілів понад 10 • 109/л і/або паличкоядерних форм понад 1,5 • 109/л) роблять діагноз пневмонії досить імовірним. Це стосується і підвищення ШОЕ понад 30 мм/год. Більш низькі цифри не виключають пневмонію, але вони нерідкі і при бронхітах.
Серед додаткових маркерів бактеріальної інфекції у діагностиці допомагає С-реактивний білок (СРБ), рівні якого понад 30 мг/л і рівні прокальцитоніну вище від 2 нг/мл дозволяють на 90 % виключити вірусну інфекцію. Однак низькі рівні цих маркерів можуть спостерігатися при пневмоніях, частіше атипових, отже, їх негативна прогностична цінність щодо діагнозу пневмонії недостатня [8].
Матеріали та методи
Дослідження проводилось у педіатричному відділенні МДКЛ № 5 у 2011–2014 рр. За чотири роки в педіатричному відділенні було проліковано 3139 дітей. У структурі захворюваності дітей, які перебували на лікуванні в умовах педіатричного відділення, питома вага дітей із ГРЗ у середньому становила 36,5 %, гострими бронхітами — 33,4 %, гострими обструктивними бронхітами — 18,1 %, з пневмоніями — 12 % дітей.
До основної групи увійшли 124 дитини віком від 1 до 7 років, більшість із них (85 %) надійшли до відділення вперше, 15 % дітей — повторно, як правило, це діти віком від 2 до 3 років життя. 30 % дітей було госпіталізовано до стаціонару на 1-шу — 2-гу добу захворювання, 48 % — на 3-тю добу, 22 % — у 1–2-й тиждень захворювання.
Результати та обговорення
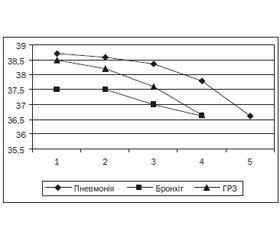
У більшості дітей захворювання розпочиналось із підвищення температури тіла до фебрильних цифр, появою кашлю, закладеності носа та виділень із нього. Тривалість і характер лихоманки залежали від нозології захворювання (рис. 1).
Підвищення температури тіла до фебрильних цифр спостерігалось у 65,5 % дітей із ГРЗ та пневмоніями, тривалість гарячкового періоду відповідно становила від 3 до 4,5 доби. Субфебрильна лихоманка була діагностована у 27,5 % дітей з ураженням верхніх дихальних шляхів і бронхітами та зберігалась протягом 3 діб. У 5,5 % дітей із ГРЗ, пневмоніями та бронхітами з обструктивним синдромом реєструвалась піретична лихоманка, тривалість якої була не більше 2 діб. В 1,5 % дітей з ураженнями органів дихання не було відзначено підвищення температури.
Аналіз анамнестичних даних дітей, які були під спостереженням, показав, що в 71,5 % випадків спостерігався ускладнений перебіг вагітності у матері, в основному через гестоз, загрозу переривання вагітності та анемію; 3,5 % вагітних хворіли на ГРЗ, у 4,5 % відзначалось загострення хронічної патології.
Характер вигодовування на першому році життя: на грудному вигодовуванні було 57,5 % дітей, на частковому грудному середнього рівня — 17,5 %, на штучному вигодовуванні — 20,5 %; 4,5 % дітей зовсім не отримували грудне молоко від народження через тяжкий стан (рис. 2).
Найбільш тяжкий перебіг захворювань органів дихання відзначався у дітей 1-ї та 2-ї груп. Обтяжений алергологічний анамнез було виявлено у більше ніж половини дітей внаслідок наявності різних видів алергозів у батьків. У кожної четвертої дитини на першому році життя відзначались алергічні реакції у вигляді шкірних висипів, свербіння, у третини дітей — прояви дисбіозу кишечника.
При первинному огляді в стаціонарі загальний стан середньої тяжкості діагностовано у 102 дітей, у 22 дітей — тяжкий стан через дихальні розлади, інтоксикацію, виражені фізикальні зміни над легенями. Кашель спостерігався у 100 % дітей. На початку захворювання він був частим, малопродуктивним. На 3-тю добу терапії кашель ставав продуктивним у 62,5 % дітей, наприкінці першого тижня захворювання він рідшав, а на 10-ту добу залишався лише у 22 % дітей. У 49,1 % дітей діагностували різні розлади дихання. Серед них задишка експіраторного характеру спостерігалась у 39 %, інспіраторна — у 42 %, змішана — у 19 % дітей.
Фізикальні зміни над легенями характеризувались жорстким диханням, при пневмонії дихання було послабленим. На фоні послабленого дихання на 3-тю — 5-ту добу від початку захворювання вислуховувались вологі дрібнопухирчасті хрипи та крепітація. При гострому бронхіті на фоні жорсткого дихання вислуховувались сухі хрипи, що в динаміці ставали вологими, різнопухирчастими. Для гострого бронхіту з бронхообструктивним синдромом характерною була наявність у 42,5 % дітей сухих хрипів із подовженим видихом, для 57,5 % — наявність вологих дрібнопухирчастих хрипів з обох легеневих сторін.
При рентгенологічному дослідженні у 75,5 % обстежених дітей виявлено посилення судинного рисунка, у 12,5 % — ознаки емфізематозу, у 12 % дітей на фоні посиленого бронхосудинного рисунка визначалась інфільтрація легеневої тканини (рис. 3).
У більшості дітей, хворих на ГРЗ, у загальному аналізі крові спостерігався лейкоцитоз, у третини хворих — через підвищення кількості нейтрофілів, в інших — через підвищення рівня лімфоцитів, а у більше ніж 30 % дітей показники крові відповідали віковій нормі. У дітей із гострими бронхітами абсолютний нейтрофільоз діагностувався у 42,5 %, абсолютний лімфоцитоз — у 35,5 %, збільшена ШОЕ — у 30,5 % дітей. При пневмонії у загальному аналізі крові у значної кількості хворих діагностувався абсолютний нейтрофільоз із зсувом лейкоцитарної формули вліво, у третини хворих — збільшена ШОЕ (рис. 4).
У дітей із тяжким і середнім ступенем перебігу пневмонії спостерігалось суттєве підвищення рівня СРБ, а також рівня прокальцитоніну вище від 2 нг/мл, що свідчило про бактеріальну етіологію процесу.
Отже, для якісної діагностики захворювань органів дихання у дітей необхідно враховувати комплекс скарг, дані анамнезу життя та хвороби, об’єктивні клінічні дані й результати параклінічних обстежень.
Висновки
1. Важливим критерієм оцінки тяжкості перебігу пневмонії слід вважати відсутність грудного вигодовування, а саме частково грудне та штучне вигодовування.
2. Діагностика ГРЗ в обстежених дітей відповідає діагностичним критеріям, затвердженим у клінічних протоколах.
3. Діагностика гострих вірусних інфекцій повинна включати клінічні прояви та параклінічні дослідження: визначення антигену вірусу у змиві з носоглотки за допомогою ІФА, виявлення антитіл до вірусу за допомогою реакції зв’язування комплементу.
4. Диференціальна діагностика вірусних і бактеріальних інфекцій дихальних шляхів повинна базуватись на визначенні рівня прокальцитоніну, вміст якого суттєво підвищується при дії бактеріальних токсинів.
Список литературы
1. Абатуров О.Є. Клінічні особливості перебігу та стан місцевого імунітету в дітей раннього віку, які хворіють на гострий обструктивний бронхіт / О.Є. Абатуров, О.О. Русакова // Перинатология и педиатрия. — 2012. — № 1(49). — С. 106-108.
2. Безрукава Л.А. Предупреждение повторных бронхообструктивных состояний у детей, перенесших респираторно-синцитиальную и аденовирусную инфекции: Автореф. дис… канд. мед. наук / Л.А. Безрукава. — Тюмень, 2009. — 21 с.
3. Заплатников А.Л. Внебольничные пневмонии у детей: принципы диагностики и этиотропной терапии / А.Л. Заплатников // Современная педиатрия. — 2010. — № 4(32). — С. 161-165.
4. Клименко В.А. Особливості перебігу гострого обструктивного бронхіту у дітей грудного віку з перинатальним ураженням центральної нервової системи / В.А. Клименко, О.В. Давиденко // Педіатрія, акушерство та гінекологія. — 2012. — № 2. — С. 19-21.
5. Мизерницкий Ю.Л. Дифференциальная диагностика и принципы дифференцированной терапии бронхообструктивного синдрома при ОРИ у детей / Ю.Л. Мизерницкий // Здоровье ребенка. — 2009. — № 1.
6. Полковниченко А.Н. Применение статистического анализа в изучении заболеваемости детей бронхолегочной патологией / Полковниченко А.Н., Гальченко В.Я., Гейвах В.С., Черепахин Ю.А. // Укр. мед. альманах. — 2010. — Т. 13, № 2. — С. 17-19.
7. Таточенко В.К. Пневмония у детей: диагностика и лечение / В.К. Таточенко // Современная педиатрия. — 2009. — № 3(25). — С. 10-11.
8. Тихомирова А.Р. Клинико-иммунологическая характеристика детей младшего возраста с бронхообструктивным синдромом: Автореф. дис… канд. мед. наук / А.Р. Тихомирова. — СПб, 2008. — 24 с.
1. O.Abaturov. Klinichni osoblyvosti perebigu ta stan miscevogo imunitetu v ditej rannogo viku, yaki xvoriyut na gostryj obstruktyvnyj bronxit. O.Abaturov, O.Rusakova. Perynatologyya y pedyatryy 2012; 1(49): 106-108.
2. Bezrukava L.A. Preduprezhdenye povtornix bronxoobstruktyvnix sostoyanyj u detej, perenesshych respyratorno-syncytyalnuyu adenovyrusnuyu ynfekcyy: avtoref. dys. na soyskanye stepeny kand.med.nauk. Tyumen 2009; 21.
3. Zaplatnykov A.L. Vnebolnychnie pnevmonyy u detej: pryncypi dyagnostyki i etyotropnoj terapyy. Zaplatnykov A.L. Sovremennaya pedyatryya 2010; 4(32): 161-165.
4. Klymenko V.A.. Osoblyvosti perebigu gostrogo obstruktyvnogo bronxitu u ditej grudnogo viku z perynatalnym urazhennyam centralnoyi nervovoyi systemy. V.A. Klymenko, O.V. Davydenko. Pediatriya, akusherstvo ta ginekologiya 2012; 2: 19-21.
5. Myzernyczkyj Yu.L. Dyfferencyalnaya dyagnostyka i pryncypi dyfferencyrovannoj terapyy bronxoobstruktyvnogo syndroma pry ORZ u detej. Zdorove rebenka 2009; 1.
6. Polkovnychenko A.N. Prymenenye statystycheskogo analyza v izuchenyy zabolevaemosty detei bronxolegochnoj patologyej. Polkovnychenko A.N., Galchenko V.Ya., Gejvax V.S., Cherepaxyn Yu.A. Ukrayinskyj medychnyj almanax 2010; 2: 17-19.
7. Tatochenko V.K. Pnevmonyya u detej: dyagnostyka y lechenye. V.K. Tatochenko. Sovremennaya pedyatryya 2009; 3 (25): 10-11.
8. Tyxomyrova A.R. Klynyko-ymmunologycheskaya charakterystyka detej mladshego vozrasta s bronxoobstruktyvnim syndromom: avtoref. dys. na soyskanye stepeny kand.med.nauk. SPb 2008; 24.
/28.jpg)

/29.jpg)