Журнал "Гастроэнтерология" Том 51, №2, 2017
Стан IgG4-позитивних плазматичних клітин у слизовій оболонці товстої кишки при хронічних запальних захворюваннях кишечника
Авторы: Yu.А. Gaidar, G.Yu. Arzhanova, A.P. Galenko
State Institution “Institute of Gastroenterology of the National Academy of Medical Sciences of Ukraine”, Dnipro, Ukraine
Рубрики: Гастроэнтерология
Разделы: Клинические исследования
Резюме
Мета роботи: вивчити стан IgG4-позитивних плазматичних клітин у слизовій оболонці товстої кишки в пацієнтів із встановленим морфологічним і ендоскопічним діагнозом неспецифічного виразкового коліту (НВК) та хвороби Крона (ХК). Матеріали та методи. У дослідженні був використаний біопсійний матеріал від 14 пацієнтів із встановленим морфологічним і ендоскопічним діагнозом НВК (8 хворих) і ХК (6 хворих) у стадії загострення, які проходили лікування в Інституті гастроентерології у відділенні захворювань кишечника. Наявність автоімунного панкреатиту I і II типу була критерієм виключення. Гістологічні препарати виготовляли стандартним методом, забарвлювали гематоксиліном та еозином. Для імуногістохімічного дослідження використовували моноклональні IgG4-антитіла (Abcam, США). Результати. Отримані результати свідчать про те, що при НВК у 37,5 % випадків не були виявлені IgG4-позитивні плазматичні клітини в слизовій оболонці товстої кишки, у 25 % випадків визначені поодинокі IgG4-позитивні плазматичні клітини, у 37,5 % виявлено групи IgG4-позитивних плазматичних клітин, але не більше 5 клітин в одній групі. При ХК спостерігались групи IgG4-позитивних плазматичних клітин, що складаються з 10 або більше клітин. Висновки. При НВК IgG4-позитивні плазматичні клітини можуть бути відсутніми, а також можуть бути поодинокими або зібраними в невеликі групи до 5 клітин у кожній. При ХК спостерігаються групи, що складаються з 10 і більше IgG4-позитивних плазматичних клітин.
Цель работы: изучить состояние IgG4-позитивных плазматических клеток в слизистой оболочке толстой кишки у пациентов с установленным морфологическим и эндоскопическим диагнозом неспецифического язвенного колита (НЯК) и болезни Крона (БК). Материалы и методы. В исследовании был использован биопсийный материал от 14 пациентов с установленным морфологическим и эндоскопическим диагнозом НЯК (8 больных) и БК (6 больных) в стадии обострения, проходивших лечение в Институте гастроэнтерологии в отделении заболеваний кишечника. Наличие аутоиммунного панкреатита І и ІІ типа являлось критерием исключения. Гистологические препараты изготовляли стандартным методом, окрашивали гематоксилином и эозином. Для иммуногистохимического исследования использовали моноклональные IgG4-антитела (Abcam, США). Результаты. Полученные результаты показывают, что при НЯК в слизистой оболочке толстой кишки в 37,5 % случаев не были выявлены IgG4-положительные плазматические клетки, в 25 % случаев определены единичные IgG4-положительные плазматические клетки, в 37,5 % случаев выявлены группы IgG4-положительных плазматических клеток, включающие не более 5 клеток в одной группе. При БК наблюдались группы IgG4-положительных плазматических клеток, состоящие из 10 или более клеток. Выводы. При НЯК IgG4-положительные плазматические клетки могут отсутствовать, а также могут быть одиночными или собранными в небольшие группы до 5 клеток в каждой. При БК наблюдаются группы, состоящие из 10 и более IgG4-положительных плазматических клеток.
Background. The diagnosis of IgG4-associated sclerosing disease, IgG4-associatied condition, is based on a comprehensive evaluation of characteristic clinical, radiographic, serologic, histological and immunohistochemical features. The histopathological is the main examination in the diagnosis of IgG4-associatied diseases. The purpose of the study was to evaluate the state of IgG4-positive plasma cells in the mucosa of the colon in patients with established morphological and endoscopic diagnosis of ulcerative colitis (UC) and Crohn’s disease (CD). Materials and methods. The study used biopsies material from 14 patients treated at the Institute of Gastroenterology, in the department intestine diseases, with established morphological and endoscope diagnosis of UC (8) and CD (6) in the acute stage. All patients had no evidence of autoimmune pancreatitis type I and II. Biopsy were fixed in 10.0% neutral formalin, dehydrated in alcohols of increasing concentration and embedded in paraffin for histological studies. Histological sections of 3–5 µm were colored with hematoxylin and eosin. There were used monoclonal IgG4 antibodies for immunohistochemical studies (Abcam, USA). Results. Our results show that with ulcerative colitis in 37.5 % of cases IgG4-positive plasma cells in the colon mucosa have not been identified. In 25 % of cases, sporadic IgG4-positive plasma cells were identified. In 37.5 % of cases, the groups of IgG4-positive plasma cells not exceeding 5 cells in one group were found. In Crohn’s disease, groups of IgG4-positive plasma cells were observed in all cases, in addition it should be noted that the group included 10 or more cells. Conclusions. It is shown that in UC, IgG4-positive plasma cells may be absent, solitary or gathered in small groups to 5 cells, and in CD, the groups consisting of 10 or more cells are observed.
Ключевые слова
IgG4-позитивні плазматичні клітини; неспецифічний виразковий коліт; хвороба Крона
IgG4-позитивные плазматические клетки; неспецифический язвенный колит; болезнь Крона
IgG4-positive plasma cells; ulcerative colitis; Crohn’s disease
Introduction
Diagnosis of chronic inflammatory bowel disease (IBD) involves two main nosologies: ulcerative colitis (UC) and Crohn’s disease (CD), and is usually based on clinical, endoscopic, radiologic, histological studies. Such diagnostics of IBD remains unchanged, despite the appearance of new technologies [1–4]. Patients with UC usually have a uniform, continuous inflammation of colonic mucosa (CM), which extends proximally from the rectum [5]. In contrast to UC, in case of CD, as a rule, there are areas of CM inflammation alternating with non-inflamed areas. One of the important histological criteria for the difference between UC and CD is the presence of granulomas. Nevertheless, granulomas are found only in 40–60 % of cases of CD in specimens of resection and much less frequently in bio–psy samples (15–36 %) [5]. In patients with IBD whose manifestations are limited to the colon and / or do not have a typical endoscopic or histological pattern, the difference between these two diseases is often difficult. Besides up to 15 % of patients with IBD are diagnosed with “undifferentiated colitis”, a term used for cases that can not be categorized as either CD or UC [6–8].
There is known the association of IBD with autoimmune pancreatitis (AIP), especially UC and AIP type I as IgG4-sclerosing disease. In fact, the diagnosis of groups of IgG4-sclerosing diseases is based on a combined assessment of typical clinical, radiologic, serological, histological and immunohistochemical characteristics. At the same time histopathological research belongs to the first place in the diagnosis of IgG4-associated diseases. The identification of three main histological signs in the affected organ allows one to precisely diagnose the disease: 1) dense lymphoplasmatic infiltrate, 2) multi-stage fibrosis and 3) obliterating phlebitis [9, 10]. The increase in the ratio of IgG4-positive plasma cells (PPC) to IgG-PPC in the affected organ increases the diagnostic significance of this sign by more than 30 % [9].
The interest in the study of the significance of IgG4-PPC tissues is now widely recognized both association for study of IBD and association of pancreatologists. Although infiltration of IgG4-PPC of the colonic mucosa is described in patients with AIP, it remains unclear now whether IgG4-po–sitive colitis exists as an independent nosological form [14].
The concentration of IgG4 immunoglobulin is known to be normally lower than that of other IgG subclasses and to be less than 5 % of the total amount of IgG in serum. An increase in the concentration of IgG4 subclass immunoglobulins in serum is detected in a number of diseases caused by infiltration of organs by plasma cells secreting IgG4. At present, allergic and autoimmune theories of the pathogene–sis of IgG4-associated diseases are discussed. The etiological relationship of AIP type I with H. pylori infection is discussed with the development of an autoimmune response to H. pylori antigens on the background of the existing deficiency of regulatory T-lymphocyte function [16]. Other authors proposed a hypothesis of the development of an excessive immune response in patients to their own microflora of the gastrointestinal tract [18]. Immunological mechanisms of AIP development are indicated by the deposition of immunocomplex deposits along the basal membranes of pancreatic acini and tubular apparatus of kidneys.
It is also known that AIP type I, seropositive form, is closely associated with an elevated serum IgG4 (over 1.35 g/l), as well as infiltration of pancreatic tissue IgG4-PPC. The detection of more than 30 IgG4-PPC in a large field of view (× 400) is known to indicate AIP type I [10]. At the same time, as the prevalence of IBD in the general population is 0.4–0.5 %, K. Ravi and co-authors diagnosed UC in 5.6 % of cases among 71 patients with AIP [11]. In another group of observation among the 85 patients with AIP there was detected IgG4-positive colitis was in 2 patients (2.4 %) [15]. Also, there were noted longer injuries and more severity of IBD in patients with AIP [12, 13].
Aim of study: to study the state of IgG4-PPC in colonic mucosa in patients with established morphological and endoscopic diagnosis of ulcerative colitis and Crohn’s disease.
Materials and methods
The study used biopsy material from 14 patients with established morphological and endoscopic diagnosis of UC (8 patients) and CD (6 patients) in the acute stage who underwent treatment in the Gastroenterology Institute in the department of intestinal diseases. The presence of signs of AIP type I and II was the exclusion criterion. For histological studies, biopsies were fixed in a 10.0 % solution of neutral formalin, dehydrated in alcohols of ascending concentration, and poured into paraffin. Histological sections 3–5 μm thick were stained with hematoxylin and eosin, and the PAS-reaction was performed. For immunohistochemical studies, rabbit monoclonal antibodies to human IgG4 (Abcam, USA) were used. The IgG4-PPC count was performed with an increase of × 400, in the zones of maximum cell concentration.
Results and discussion
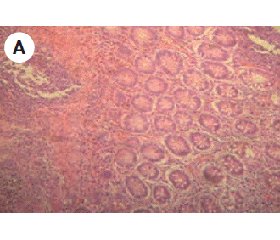
The results of our studies showed that in patients with UC in 37.5 % of cases IgG4-PPC in CM were not detected (fig. 1).
In 25.0 % of cases there were detected single IgG4-PPC (fig. 2).
In 37.5 % of cases there were detected groups of IgG4-PPC not exceeding 5 cells in one group (fig. 3).
As for CD, in this disease groups of IgG4-PPC were observed in all cases studied by us, besides it should be noted that the groups included 10 or more cells (fig. 4).
In our study there were shown the morphological features of IgG4-PPC localization in CM in patients with UC and CD. These results may indicate the involvement of autoimmune mechanisms in the development of IBD. It is known that in the normal state there are no IgG4-PPC in organs and tissues. The fact that IgG4-PPC were not detected in 37.5 % of patients with established diagnosis of UC may indicate mild forms of the disease. At the same time, in 62.5 % of patients with the same diagnosis we observed single IgG4-PPC or a group of cells, which in turn may indicate the severity of the course of the disease.
In conclusion, we would like to draw your attention to the fact that immunohistochemical detection of IgG4-PPC in CM helps to search for diagnostic differences between UC and CD.
Conclusions
1. The determination of IgG4-PPC in CM allows one to recognize IgG4-positive (up to 5 IgG4-PPC at large field of view) and IgG4-negative form (0 IgG4-PPC at large field of view) in patients with UC.
2. The immunohistochemical detection of IgG4-PPC in CM can help in creating a distinction between UC and CD (more than 10 IgG4-PPC at large field of view in patients with CD).
3. The obtained results testify to the involvement of IgG4-PPC in the pathogenesis of chronic IBD.
Conflicts of interests. Authors declare the absence of any conflicts of interests that might be construed to influence the results or interpretation of their manuscript.
Список литературы
1. Adler G. Bolezn Krona i yazvennyiy kolit [Crohn’s disease and ulcerative colitis]. Мoscow: GEOTAR Media; 2001. 500p. (in Russian)
2. Belousova EA. Yazvennyiy kolit i bolezn Krona [Ulcerative colitis and Crohn’s disease]. Tver: Triada; 2002. 128 p. (in Russian)
3. Halif IL, Loranska ID. Vospalitelnyie zabolevaniya kishechnika (nespetsificheskiy yazvennyiy kolit i bolezn Krona). Klinika, diagnostika i lechenie. [Inflammatory bowel disease (ulcerative colitis and Crohn’s disease). The clinic, diagnosis and treatment]. Мoscow: Miklosh; 2004. 88 p. (in Russian)
4. Stepanov YuM, Stoykevich MV, Sorochan OV. Application of 5-Aminosalicylic Acid Preparations in the Treatment of Inflammatory Bowel Diseases. Hastroenterolohiya. 2016;3(61):80-88. doi: 10.22141/2308-2097.3.61.2016.79163. (in Ukrainian)
5. Stepanov YuM, Gaydar YuA. Immunoglobulin G4-associated sclerosing disease of the digestive system. Vesnik akademii meditsinskih nauk Ukrainyi. 2015;21(1):54-60. (in Russian)
6. Silverberg MS, Satsangi J, Ahmad T, et al. Toward an integrated clinical, molecular and serological classification of inflammatory bowel disease: report of a working party of the 2005 Montreal World Congress of Gastroenterology. Can J Gastroenterol. 2005 Sep;19 Suppl A:5A-36A. PMID: 16151544.
7. Schukina OB. Indeterminate colitis: current status of the problem. Consilium Medicum Ukraina. 2009;3(7):3-5. (in Russian)
8. Stoykevich MV. Effect of Nutritional Status Disorders on the Quality of Life in Patients with Chronic Inflammatory Bowel Diseases. Hastroenterolohiya. 2016;1(59):77-81. doi: 10.22141/2308-2097.1.59.2016.74532. (in Ukrainian)
9. Deshpande V. The pathology of IgG4-related disease:critical issues and challenges. Semin Diagn Pathol. 2012 Nov;29(4):191-6. doi: 10.1053/j.semdp.2012.08.001.
10. Sato Y, Notohara K, Kojima M, Takata K, Masaki Y, Yoshino T. IgG4-related disease: historical overview and pathology of hematological disorders. Pathol Int. 2010 Apr;60(4):247-58. doi: 10.1111/j.1440-1827.2010.02524.x.
11. Virk R, Shinagare S, Lauwers GY, Yajnik V, Stone JH, Deshpande V. Tissue IgG4-positive plasma cells in inflammatory bowel disease: a study of 88 treatment-naive biopsies of inflammatory bowel disease. Mod Pathol. 2014 Mar;27(3):454-9. doi: 10.1038/modpathol.2013.121.
12. Ravi K, Chari ST, Vege SS, et al. Inflammatory bowel disease in the setting of autoimmune pancreatitis. Inflamm Bowel Dis. 2009 Sep;15(9):1326-30. doi: 10.1002/ibd.20898.
13. Gaidar YA, Oshmyanska NY, Halenko A.P. Histostructure of pancreas in patients with autoimmune pancreatitis type I and II: connection with the level of IgG4-positive plasma cells. Patologiya. 2014;30:68-71. (in Russian)
14. Bueverov AO, Kucheriavyi YA. IgG4-assotsiirovannaia bolezn’: monografiia [IgG4-associated disease: a monograph]. Moskow: Forte Print; 2014. 128 p.
15. Kuwata G, Kamisawa T, Koizumi K, et al. Ulcerative colitis and immunoglobulin G4. Gut Liver. 2014 Jan;8(1):29-34. doi: 10.5009/gnl.2014.8.1.29.
16. Guarneri F, Guarneri C, Benvenga S. Helicobacter pylori and autoimmune pancreatitis: role of carbonic anhydrase via molecular mimicry? J Cell Mol Med. 2005 Jul-Sep;9(3):741-4. PMID: 16202223.
17. Akitake R, Watanabe T, Zaima C. Possible involvement of T helper type 2 responses to Toll-like receptor ligands in IgG4-related sclerosing disease. Gut. 2010 Apr;59(4):542-5. doi: 10.1136/gut.2009.200972.
18. Deshpande V, Chicano S, Finkelberg D, et al. Autoimmune pancreatitis: a systemic immune complex mediated disease. Am J Surg Pathol. 2006 Dec;30(12):1537-45. doi: 10.1097/01.pas.0000213331.09864.2c.

/26-1.gif)
/27-1.gif)