Журнал «Здоровье ребенка» 1 (60) 2015
Вернуться к номеру
Gastrointestinal food allergy in the children as the up-to-date issue
Авторы: Okhotnikova O.M., Gladush Y.I., Fedushka H.M., Pidvyshenna T.V., Borovik Y.R., Bondarenko L.V., Ukrainska T.L., Pidgirna N.V., Shestakova O.S., Zarudna O.F., Gritshenko O.M. - P.L. Shupyk National Medical Academy of Postgraduate Education
Рубрики: Педиатрия/Неонатология
Разделы: Справочник специалиста
Версия для печати
Foreword:
Diagnosis of various clinical manifestations which developing on the food, mainly in childhood, is topical issue nowadays. Food allergy is undesirable reaction to foods with proven immune mediated mechanism, the basis of clinical manifestations which are IgE-like-dependent, so i IgE-independent immune reaction and their combinations. It clinically manifested by skin, respiratory and gastrointestinal syndromes. Prevalence of food allergy varies in the range - up to 6-8% of children. The main part research is dedicated to the study of only frequently used products, so its true prevalence is difficult to determine.
The genetic predisposition is a prerequisite for the development of food allergy. Important clinical characteristic of food allergy are recurrent, prolonged and chronic current. Because of this is, there are frequent exacerbations and further development of “allergic march”. There are proteins that stimulate in genetically predisposed children activation of Th2-helper cells and stimulate the production of IgE-antibodies, and can penetrat the barrier of the gastrointestinal tract and enter into contact with the immune cells in the internal environment of the organism. These proteins are etiologically important allergens of the food.
The relationship of food allergy and atopic dermatitis is important question. Disorder of morpho-functional state of the digestive system is the main reason for the emergence mechanism for food allergy. Children with functional bowel disorders prone to the development food allergy. Gastrointestinal symptoms of food allergy in infants occur during the introduction of complementary foods. At the age of 6 years, more than half of the children already diagnosed chronic diseases of the digestive system, the connection of which with food allergy remains unrecognized.
Goal of research: proper investigation of the gastrointestinal form of the food allergy among the children with allergic and somatic pathologies.
Patients and methods of research. We have examined 106 children. Basic group: 60 patients (age from 1.5 to 17 years) with various manifestations of allergy. Group of comparison: 46 children with different somatic pathology of digestive system. Clinical, laboratory (total Ig E) and endoscopic, morfological studies were conducted.
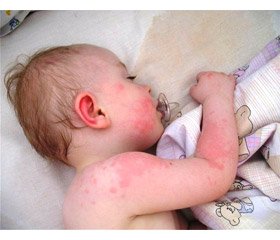
Results of research. The allergy was mostly caused by the cow milk protein (22), citrus fruit (10), chocolate (9) and strawberries (8). The patients had various allergic reactions: skin dryness, fissures, scratching, dermahemia, erythematic and squamosal foci, infection, papular rash, macular and papular rash, scabs. In most cases the rash covers the whole body – 30% (n=18) of children, 16,7 % (n=10) have rash on the face and around the mouth; also rash affects feet, ankles and hips in 16,7% (n=10) of cases; and 13,3% of patients (n=8) have rash on their hands. Gastrointestinal problems may be divided into several groups – pain syndrome, diarrheal disease, asthenic and vegetative diseases. In the process of abdominal palpation, we observed the pain in epigastrium (35%), Kerr spot (31,6%), Chauffard zone (5%), periumbilical area (10%), pyloroduodenal area (20%), intestine area (3,3%), Ortner syndrome(6,7%). 17 children did not feel any pain in the course of examination (28%). 10,7% of children of the 1st group and 15,6% of children of the 2nd group had nausea, 0% and 12,5% had heartburn and 10,7% and 18,75 had small appetite.
Abdominal distension was observed among 8,3% of children. 13,3±8,7% had moderate hepatomegaly. Defecation among the children with gastrointestinal allergy has the following characteristics: formed stool – 76,7±10,9%, constipation - 18,3%, diarrhea – 5%. Eosinophil quantity (4,6±0,6%) is distinct among 61,7% of children, 40,5% have over 5% of eosinophils. According to the data received by esophagogastroduodenoscopy, the motor activity is characterized by abnormalities of the motor activity in stomach, esophagus and duodenum, mostly due to reflux. In the first group 67% of children have normal cardiac interlocking, 25% have incomplete cardiac interlocking, 5% have gastric mucosa prolapse, 30% have bile in the stomach. In the 2nd group 87% of children have normal cardiac interlocking, 0% have incomplete cardiac interlocking, 6,5% have gastric mucosa prolapse, 30% have bile in the stomach. Incomplete interlocking of the cardia plays important role during the diagnostic of food allergy (χ2(1) = 14,095, φ = 0,374 which shows the medium relation). While comparing of the visual changes of the mucosa (lymphoid elements, incrustation in the form of manna grouts) of the esophagus, stomach and duodenum showed no significant relationship between main patients group and group of compare (χ2 does not exceed the critical score). There were combinations of bronchial asthma, allergic rhinitis and dietary allergy with normal IgE, which is due to the participation of various immune mechanisms not only IgE-mediated.
Conclusions. Among the children who had various allergic reactions and gastrointestinal diseases, we managed to find the provocative allergen in 67% of cases. Allergic diseases are characterized by a significant (by 3-5 times) increase of the level of the total serum IgE. Absence of eosinophil’s does not mean the absence of allergy. Esophagogastroduodenoscopy and morphological study may be used in the differential diagnosis of allergic (lymphoid hyperplasia) and non-allergic damage of gastrointestinal mucosa, the indications for their active detection are the presence of the burdened familial history and allergic diseases in children.
1. Balabolky`n Y`.Y`. Kly`ny`ko-y`mmunology`chesky`e vary`anty atopy`cheskogo dermaty`ta u detej y` podrostkov y` эffekty`vnost` patogenety`cheskoj terapy`y` [Tekst] / Y`.Y`. Balabolky`n, T.E. Sady`kova// Pedy`atry`ya. – 2013. - Tom 92, # 3. – S. 6-13.
2. Bely`czkaya M.Yu. Osobennosty` techeny`ya gastroy`ntesty`nal`nogo sy`ndroma u detej pervogo goda zhy`zny`, naxodyashhy`xsya na estestvennom vskarmly`vany`y` [Tekst] / M.Yu. Bely`czkaya,T.B. Senczova, S.N. Deny`sova, Y`.Ya. Kon`y` dr. // Rossy`jsky`j vestny`k pery`natology`y` y` pedy`atry`y`.- 2010.- # 5.- S. 45-51.
3. Borovy`k T.E.Mexany`zmы razvy`ty`ya py`shhevoj allergy`y` [Tekst] / T.E. Borovy`k, S.G. Gry`baky`n, S.G. Makarova y` dr. // Pedy`atry`ya. - 2011. – Tom 86, # 4. – S. 128-134.
4. Volosovecz A.P. Teorety`cheskoe obosnovany`e preventy`vnoj roly` ky`shechnoj my`kroby`otы v geneze allergy`chesky`x zabolevany`j u detej [Tekst] / A.P. Volosovecz, S.P. Kry`vopustov, N.T. Makuxa y` dr. // Dy`tyachy`jlikar. - 2013. - # 4 (25). – S. 5-8.
5. Deny`sova S.N. Dy`etoterapy`ya gastroy`ntesty`nal`nogo sy`ndroma u detej s atopy`chesky`m dermaty`tom [Tekst] / S.N. Deny`sova // Lechashhy`j vrach. - 2012. - # 4. - S. 54-55.
6. Kaznacheeva L.F. Gastroy`ntesty`nal`naya forma py`shhevoj allergy`y` u detej [Tekst] / L.F. Kaznacheeva // Prakty`cheskaya medy`cy`na.- 2010.- # 45.- S.88-92.
7. Klykova T.V. Py`shhevaya allergy`ya u detej rannego vozrasta: podxodы k dy`agnosty`ke y` lecheny`yu [Tekst] / T.V. Klыkova, E.V. Agafonova, Y`.D. Reshetny`kova // Prakty`cheskaya medy`cy`na.- 2011.- # 51.- S. 125-131.
8. Kruhlova L.S.Symptomokompleks dysbyoza u bol'nykh atopycheskym dermatytom y metodi eho korrektsyy [Tekst] / L.S. Kruhlova // Lechashchyy vrach. – 2012. - # 5. – S. 38-44.
9. Macharadze D.Sh. Atopycheskyy dermatyt y pyshchevaya allerhyya. Chto obshcheho? [Tekst] / D.Sh. Macharadze// Lechashchyy vrach. – 2013. - # 5. – S. 24-30.
10. Okhotnykova E.N. Hastroyntestynal'naya pyshchevaya allerhyya u detey [Tekst] / E.N. Okhotnykova // Klinichna imunolohiya. Alerholohiya. Infektolohiya.- 2013.# 2. - S. 5-13.
11. Okhotnykova E.N. "Allerhycheskyy marsh": svyaz' pokolenyy y эskalatsyyaallerhyy u detey[Tekst] / E.N. Okhotnykova // Klinichna imunolohiya. Alerholohiya. Infektolohiya. – 2008. - # 4 (15). – S. 7-15.
12. Revyakyna V.A. Pyshchevaya allerhyya, hastroyntestynal'nye proyavlenyya [Tekst] / V.A. Revyakyna // Lechashchyy vrach. – 2013. - #4.–Ts. 13-17.
13. Sazonova N.E. Porazhenye verkhneho otdela pyshchevarytel'noho trakta u detey doshkol'noho vozrasta s atopycheskym dermatytom y hastroyntestynal'nыmy proyavlenymy pyshchevoy allerhyy [Tekst] / N.E. Sazonova, E.Y. Shabunyna, N.Yu. Shyrokova y dr. // Pedyatryya. – 2013. – Tom 92, # 3. – S. 13-17.
14. Blzquez A.B., Mayer L., Berin M.C. Thymic stromal lymphopoietin is required for gastrointestinal allergy but not oral tolerance [Теxt] / A.D. Bl?zquez, L. Mayer, M.C. Berin // Gastroenterology.- 2010.- Vol. 139 (4).- P.1301–1309.
15. Bol-Schoenmakers M., et al. Regulation by intestinal gd T cells during establishment of food allergic sensitization in mice [Теxt] / [published online ahead of print September 29, 2010] // Allergy. - 2010.- P.02479.x
16. Can We Produce true Tolerance in Patients With Food Allergy? [Text] / M.C. Berin, L. Mayer // J. Allergy Clin. Immunol.- 2013.- Vol.131, Issue 1.-P. 14-22.
17. Food allergy [Text] / S.Р. Sicherer, H.A. Sampson // J. Allergy Clin. Immunol. – 2010.-Vol.125,Issue 2, Suppl. 2.-P. S354.
18. Mechanisms of Immune Tolerance Relevant to Food Allergy [Теxt] / B.P. Vickery, A.M. Scurlock et al. // J. Allergy Clin. Immunol. - 2011. - Vol. 127 (3). - P. 576–586.
19. Ostblom E., Lilja G., Pershagen G., van Hage M., Wickman M. Phenotypes of food hypersensitivity and Development of Allergic Diseases During the First 8 Years of Life [Теxt] / E. Ostblom, G. Lilja et al. // Clin Exp Allergy.- 2008.- Vol. 38.- P.1325-1332.
20. Robison R.G. Food Allergy [Теxt] / R.G. Robison, J.A. Pongracic // Allergy Asthma Proc.- 2012.- Vol. 33, №3. – P. 77-79.